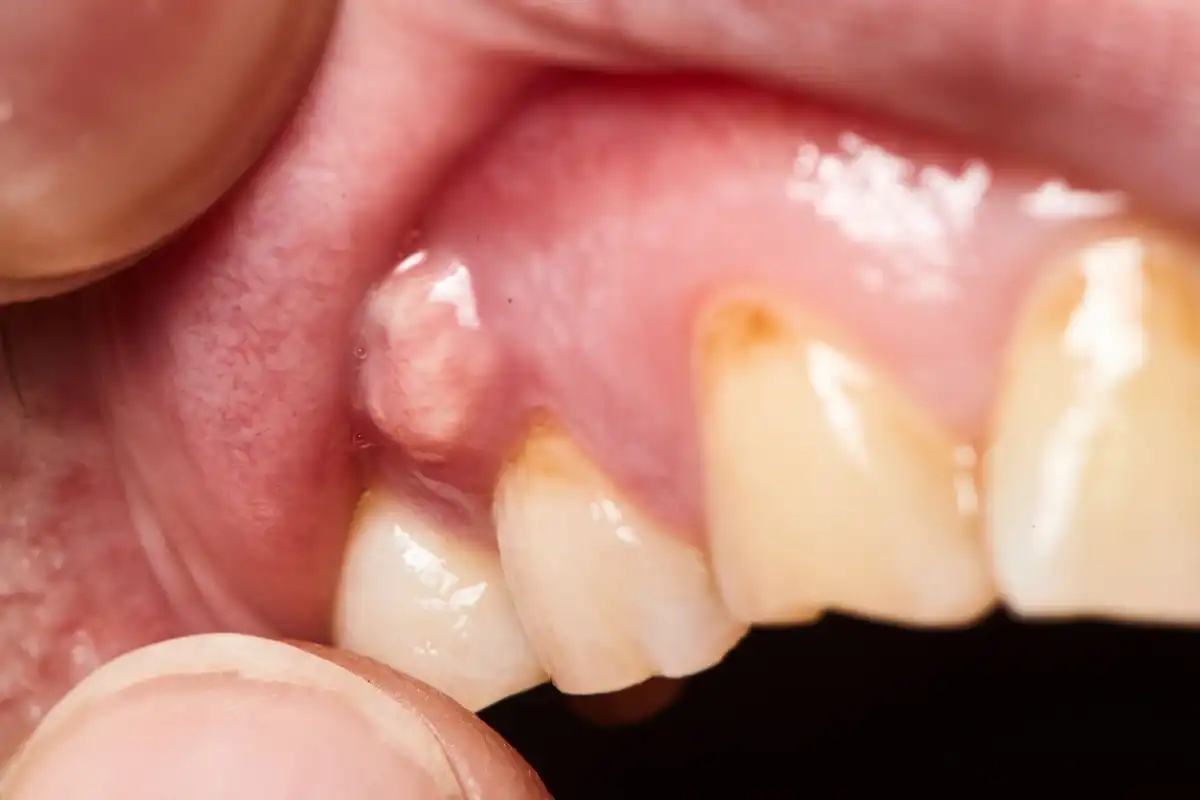
Gum Disease: Symptoms, Treatment, and Risks


Gum disease – aka “periodontitis” aka “periodontal disease” – is the most common reason behind adult tooth loss. Not cavities, not accidents or dental emergencies…gum disease.
No matter how healthy you keep your teeth, your mouth depends on healthy gum tissue (gingiva) to help anchor and support your tooth roots. If you don’t have healthy teeth and gums, the bone underneath them (which is also responsible for supporting your teeth) won’t be healthy either.
And to make matters even worse, science now shows us that having gum disease can seriously raise your risk of health problems.
Causes Of Gum Disease?
1) Oral Biofilm
Dental plaque is ultimately the main cause of gum disease. When you don’t brush or floss good enough, all of that bacteria hangs out along your gumlines and creeps under the gum tissue. Within a week or so you’ll start to see swelling and redness.
2) Hormone Imbalance
Pregnancy gingivitis and the occasional monthly gum swelling when you get your period are common for some women. But don’t brush off your gum disease on hormones; make sure you’re still practicing good oral hygiene.
3) Medical Or Health Issues
People with certain types of health problems are more prone to getting gum disease because of the strain to their immune system. Diabetes is one example. Since oral biofilm feeds off of sugars, irregular blood glucose levels can add to your chances of periodontitis.
4) Genetics
Does gum disease run in your family? You might be more predisposed to it, especially since bacteria can spread when you’re sharing eating utensils or kissing. Fortunately, good oral health hygiene and preventative care can reduce your chances of getting gum disease, if not prevent you from getting it at all.
5) Tobacco Products
The increased risk factors of gum disease from dip and tobacco can cover up the symptoms and mask infection, allowing it to reach severe stages before you know there’s even a problem. Gum disease from dip is quite common. Since tobacco products dry out your gingiva and slow blood flow, it’s harder for your teeth and gums to stay healthy.
Gum Disease Symptoms
- bad breath
- teeth and gums sensitive
- tender gum tissue
- bleeding when you brush or floss
- gum recession
- spaces between teeth
- teeth that are loose or shifting
- soreness when you bite down
- changes in how your teeth bite together
Take note: if you smoke or use tobacco products like dip, you might not notice any bleeding, swelling, or redness. That’s why it’s so important to schedule regular screenings with a dentist before a more aggressive form of gum disease, periodontitis kicks in.
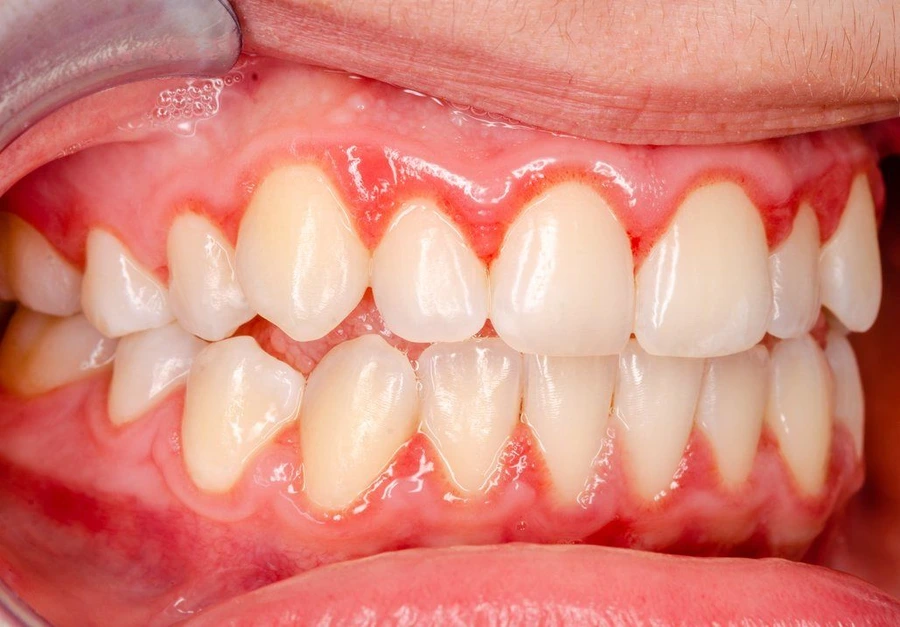
To get a firm answer as to whether you have gum disease or not, your dentist or dental hygienist will use a special measuring tool called a periodontal probe to see how deep the “pockets” are under your gum tissue. The deeper they are, the less tissue is attached to your tooth. X-rays will also show how much bone loss there is.
Gum Disease Treatment
The best treatment for gum disease is therapy that starts as soon as possible. The longer you wait, the more the gums and bone will deteriorate (and they can’t be regrown). If your gum disease becomes severe, it can be treated and managed by a dental specialist known as a periodontist. Here are some of the different types of therapies that are used:
1) Periodontal Scaling & Root Planing (Aka “Deep Cleaning”)
2) Periodontal Maintenance Cleanings
After your deep cleanings are completed, you’ll want to see the hygienist for maintenance cleanings every 3-4 months to prevent relapse of symptoms. At some point, they might place you back onto a regular prophylaxis (cleaning) schedule or keep you on this cycle for the long term.
3) Locally Placed Antibiotics
Severely infected gum pockets can be harder to treat. Small antibiotic capsules can be placed down into these areas to release tiny particles of medication over the course of a week to help speed up recovery.
4) Bone Or Gum Grafts
To avoid an extraction, your dentist might be able to add to the supportive tissues around your tooth by placing a graft. These treatments are usually reserved for more aggressive periodontal disease.
What's The Difference Between Gingivitis And Periodontitis?
Both gingivitis and periodontitis are different stages of gum disease. On one end you have gingivitis, which is the initial stage of inflammation and redness. What you need to know is that gingivitis is still completely reversible. But once it gets to the point where tissue is detaching from the teeth and the bone starts shrinking around your roots, you’ve entered into the stage of gum disease that’s full-fledged periodontitis.
BONUS: What does periodontitis mean? We’ll break it down for you:
Perio = around
Dont = tooth
Itis = inflammation of
In other words, periodontitis is inflammation around your tooth.
Periodontitis is a form of gum disease that has different stages, ranging from mild to severe. Mild periodontal disease is minimal pocketing under the gums and mild bone loss. Moderate gum disease is more aggressive tissue deterioration and loss, with pockets up to 5-7mm deep. Severe periodontitis involves tooth mobility and loss because of such aggressive structural damage and pockets over 7mm deep.
Gum Disease Prevention
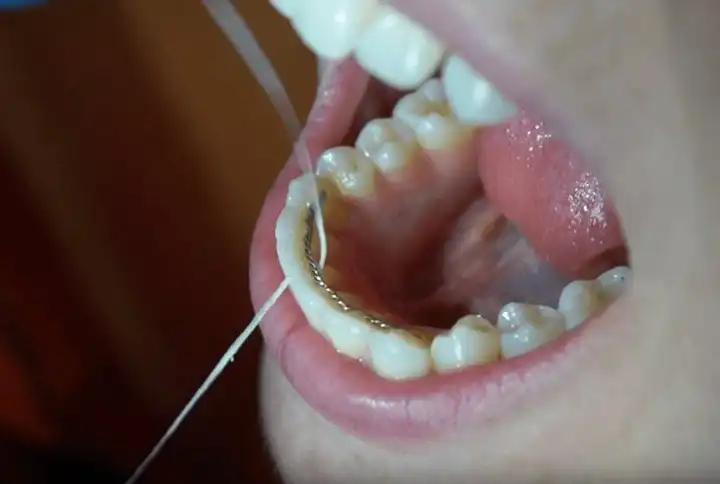
Since plaque creeps under the gumlines, you’ll need a way to clean those areas too. Wrap your floss tightly in a “C” around each tooth, sliding up and down each side to clean out the pockets under your tissue. As long as you only have the beginning stages of gingivitis, any bleeding should go away within about two weeks if you’re flossing every day. Can’t floss? Consider getting a water flosser to help.
Be sure to schedule a regular preventative cleaning (aka prophylaxis) at least every six months to clean off any buildup that you may have missed. Even if you’re great at brushing and flossing, most people do see some tartar accumulation in hard-to-reach areas or around their saliva glands.
Related Health Issues With Gum Disease
If losing your teeth to gum disease wasn’t scary enough, there are more risk factors at play here. Research shows and proves that severe periodontal infections directly increase your chances and severity of:
- heart disease and heart attack
- high blood pressure
- stroke
- pneumonia
- diabetes
- infertility
- erectile dysfunction
- preeclampsia
…and possibly even Alzheimer’s disease and dementia. The great news is that those same scientific studies tell us that by improving your gum health and treating periodontitis, you can have a positive impact on your overall level of wellness.
Gum Disease Recap
Gum disease is one of the most common oral health infections and the leading cause of adult tooth loss in the United States. It’s also preventable, but only if you catch it in the earliest stage of gingivitis. Once more aggressive periodontal disease kicks in, you’ll require professional treatment to prevent tooth loss.
The severity of your gum disease can put your health at risk. As medical issues and periodontitis go hand in hand, it’s crucial to treat them together instead of as two separate issues.
Treating gum disease starts at home with good daily oral health habits by brushing and flossing, followed up with professional cleanings with your hygienist.
Make your inbox smile!
Subscribe