Why Are My Gums Swollen? | Causes, Treatment, & Prevention

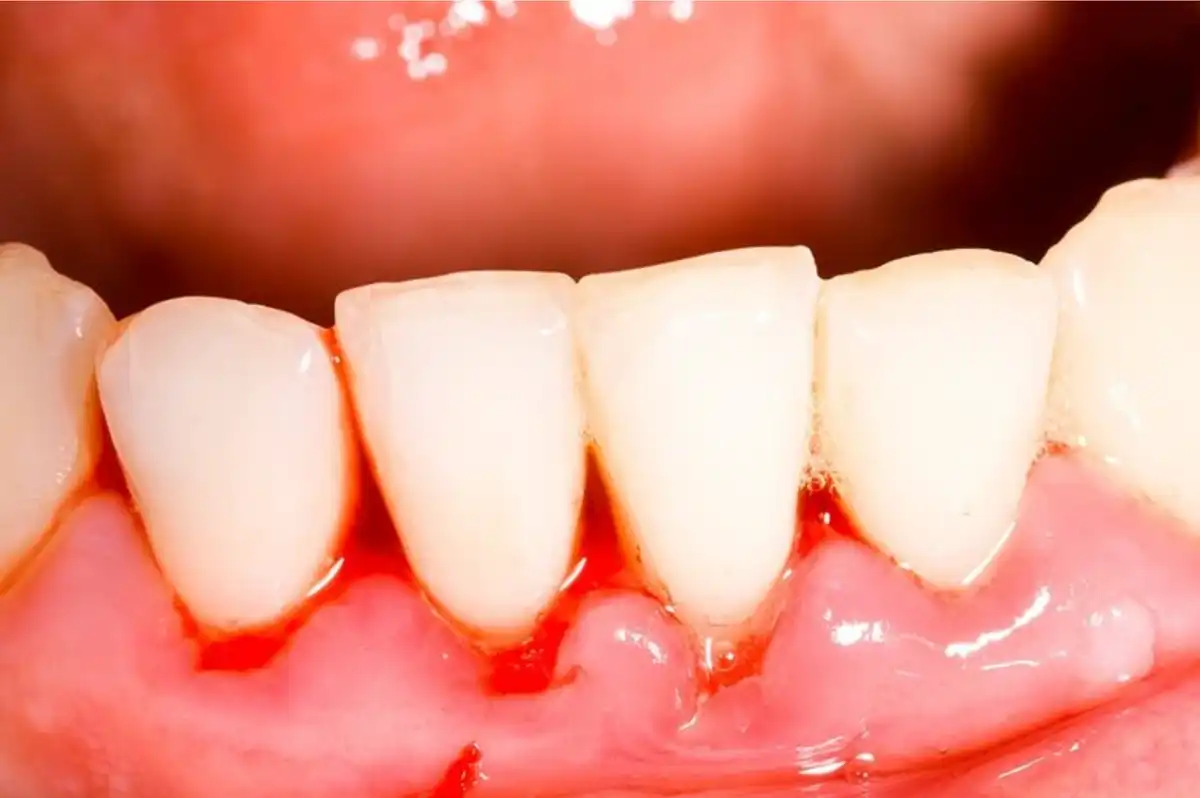
Are you someone who tends to get swollen gums? Inflammation and redness, particularly along the edges of your gums near your teeth, is called “gingivitis”. We use the word “-itis” to describe “inflammation of” something. In this case, is your gingiva (gum tissue.) Swollen gums around teeth can range from mild gingivitis to more aggressive periodontal disease. Severe infections typically involve painful, swollen gums, as well as the loss of tooth support.
Understanding how to treat swollen gums can help you promote better overall health, but also save your smile for the years to come!
Swollen Gums Common Symptoms
Swollen gums around teeth are pretty easy to identify. They tend to be puffy looking and possibly even “smooth” or “shiny” on the surface, as the tissues are stretched out from all of the inflammation. Depending on the severity of your swollen gums, your gums might be sensitive to touch. Although you’re probably not putting your hands in your mouth, you’ll notice the irritation when you’re brushing or flossing. They might even hurt when you chew food.
When you have swollen gums it’s also common to see bleeding. Any time your gums are stimulated, they may start to bleed. This is especially noticeable when you’re brushing and flossing. Most people assume that flossing is what makes their gums bleed. In reality, it’s the lack of flossing that contributes to it. All of the plaque accumulating along the edges of your gums trigger an immune response. And what do you get? Swollen gums!
If you don’t know how to treat swollen gums, the inflammation and disease process can easily progress into something worse. Over time the tissues start to detach from your teeth and recede. When that happens, it exposes the roots of your teeth, making them prone to sensitivity and decay. Ultimately the bone will also resorb (shrink) and lead to a lack of tooth support. At that point, people with gum disease will also start to experience tooth mobility or their teeth may even fall out.
Causes For Swollen Gums
1) Gingivitis
If you have swollen gums, it’s almost always due to gingivitis. After all, gums = “gingi-” and swelling = “-itis”. This condition will be one of the first things your dentist wants to rule out if you’re complaining of painful swollen gums. The swelling is caused by bacterial deposits next to your gums, due to inadequate oral hygiene.
Symptoms
Common signs of gingivitis include swelling, sensitive gums, redness (particularly along the edges of teeth), and bleeding when you brush and floss. You might even notice a glossy appearance where the tissues are swollen the most. Swollen gums are easy to spot along the gum line.
Treatment
2) Periodontitis Or Gum Disease
If gingivitis isn’t cured, it will gradually progress into a more serious form of gum disease known as periodontitis. At this point, the gum swelling isn’t something you can simply reverse with good oral hygiene. Rather, you’ll need to seek out the care of your dentist in order to avoid tooth loss. Unfortunately, periodontal disease can also raise your risk of heart disease, stroke, diabetes, pneumonia, and many other medical conditions.
Symptoms
Treatment
Periodontal treatment varies depending on the extent of your infection. A deep cleaning is usually required for gum disease. For aggressive gum disease, your dentist might also recommend medication or tissue grafting. If a tooth is severely infected, it may need to be extracted. The earlier treatment is initiated, the less likely the infection is to spread to other areas of your mouth.
3) Infection
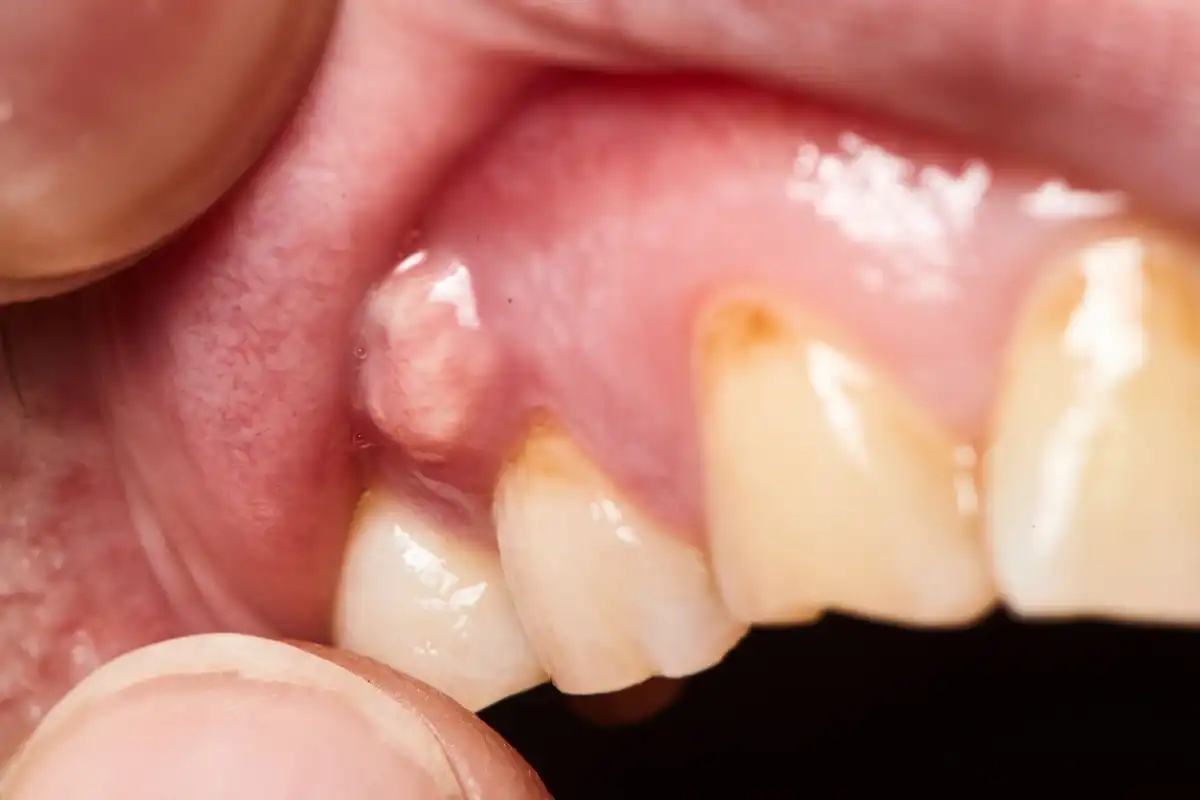
Your mouth is a reflection of your overall health. If there is redness or swelling and your dentist has ruled out gingivitis/gum disease, it could be linked to an underlying medical condition that’s yet to be diagnosed. Recognizing the signs of irregular gum swelling could indicate that your body is fighting off some bigger type of infection that requires your attention.
Symptoms
Depending on the type of infection that you have, you’ll probably also notice issues like raw swollen gums, red tissues inside of your mouth, white patches or spots, changes in your taste sensations, or a fever. Infections like thrush also tend to cause bad breath or pain while you’re swallowing.
Treatment
Most treatments for an oral infection focus around maintaining a clean environment (including any removable prosthetics) and some type of medication, whether it’s an anti-fungal, antibiotic, steroid, etc. The best treatment will depend on what it is that’s causing the infection. If it’s due to a systemic condition, you may need a referral to your primary care physician to have bloodwork done.
4) Pregnancy Gingivitis
Some women never experience oral health problems until they’re pregnant. Nausea and vomiting may lead to changes in appetite or oral hygiene habits, allowing swollen gums to develop. Hormones also play a role, as they can often lead to pseudo-gingivitis and swelling along the gums. Since actual gum disease is linked to premature labor, preeclampsia, and low birth weights in infants, it’s important to address symptoms and rule out aggressive infections.
Symptoms
Treatment
If the gingivitis is due to changes in diet and oral hygiene, a professional cleaning and re-vamped home oral care routine are the best treatment. For true “pregnancy gingivitis” or tissue overgrowth, time may be the only answer. In some cases, large areas of excess tissue can be removed by the dentist (if they are interfering with everyday activities or are a serious aesthetic concern.)
5) Tobacco Products Or Vaping
Any time you’re using tobacco products, e-cigs, or other types of vaping agents, you put yourself at risk for tissue burns. Usually, you’ll see white or red patches in the roof of your mouth (you’ll need a mirror.) Because of the high temperatures and isolated exposure, smoking and similar types of activities can irritate your gums and make it difficult for them to heal.
Symptoms
Treatment
Work with your dentist on developing a smoking cessation plan. Giving up tobacco products can help your mouth heal more quickly and lower your chances of additional oral infections. And since tobacco products tend to cover up the most common signs of swollen gums, quitting is an important step in having a healthier mouth.
6) Canker Sores
From time to time, most of us are affected by the occasional canker sore. In some individuals, underlying viruses can also contribute to recurring cold sore ulcers. If you’re someone who has a sudden and specific area where the gums are swollen, it could be due to these seemingly harmless — although bothersome — oral sores.
Symptoms
Canker sores tend to look like small circular areas that are red or white. You’ll usually be able to see a border around the edge. The ulcer will be tender to touch. It’s important to rule out an abscess, so make note of where it’s located. Irritants such as foods or orthodontic appliances may be enough to rub your gums and create an ulcer, so trying to rule out the causes is one of the best ways to prevent flare-ups.
Treatment
A typical canker sore will usually just need to run its course. For most individuals, ulcers last about a week. Cold sores can take up to 10-14 days to fully heal. If the ulcer is due to a virus or you have frequent flare-ups, ask your dentist for a prescription. Otherwise, keep the area clean, rinse with warm saltwater routinely, and address any irritants in that area.
7) Malnutrition
Although less common, cases of malnutrition or an existing eating disorder can contribute to red inflamed gums or something people refer to as “scurvy.” People with missing teeth, ill-fitting dentures, and gastrointestinal problems tend to have difficulty absorbing the right nutrients and may exhibit signs of malnutrition, as well as children who may not have access to nutrient-dense foods. Malnutrition can lower your body’s resistance to plaque biofilm and slow your ability to heal. Malnutrition may be a concern for older or physically impaired individuals who have difficulty eating or are on a restrictive diet.
Symptoms
Malnutrition can exhibit itself in the oral environment as red gums and higher caries (decay) levels. It can also cause saliva gland dysfunction, delayed tooth eruption, a swollen tongue, cracked lips, burning mouth syndrome, and smaller tooth size. Along with bleeding gums, oral infections tend to take longer to respond to treatment. Your dentist can also observe changes in the bone structure on your dental X-rays.
Treatment
Preventing Swollen Gums
Thankfully it’s easy to prevent swollen gums around teeth. It all boils down to a great daily oral hygiene routine. By thoroughly removing plaque biofilm along your gum line each day, you’re eliminating the source of the infection. After about 2-3 weeks, all signs of mild to moderate gingivitis should be almost — if not completely — eliminated.
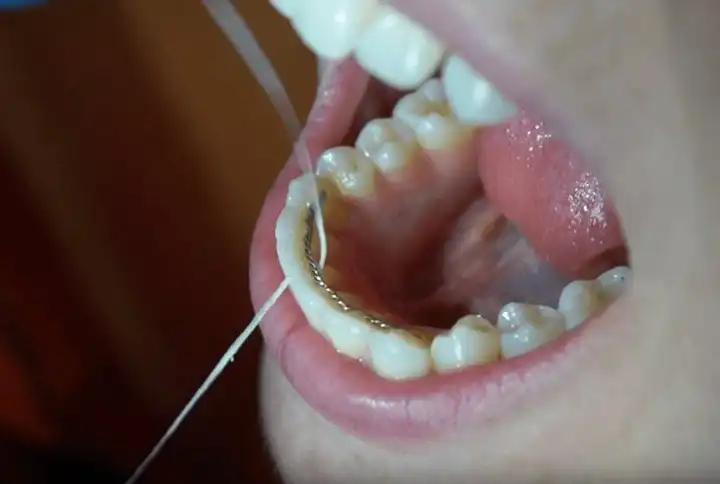
First and foremost, flossing is key if you want to reduce gum swelling. When you floss it’s particularly important to hug the strand tightly against the side of your tooth in a “C” shape, to conform to all of the curves. The second most important thing to do is to make sure you’re sliding the floss up and down just under the edges of your gums. Don’t worry, you’re not going to hurt them! What you’re trying to do is to disrupt the bacteria that have settled along and just underneath the edges of your gums in what we call the “sulcus” or “pocket.” Once you’ve cleaned one tooth, lift the floss up and over your gums then move to the next one.
When you brush, do your best to angle the bristles by about 45-degrees towards your gum tissues. This helps to stimulate your gums and remove plaque so that they heal quicker. Always use soft bristles, short strokes, and light pressure. If you scrub too hard it can make your gums recede!
Soothing Painful Swollen Gums
What’s the best treatment for relieving painful, swollen gums? Aside from cleaning the area to naturally get the infection to go away (the brushing and flossing we talked about) you can also:
- Rinse with warm saltwater to naturally draw out inflammation.
- Take an anti-inflammatory, such as ibuprofen (Motrin).
- Apply a few drops of clove oil with a cotton swab or Q-tip.
Unless the bacteria that are causing your swollen gums are removed, you won’t be able to get rid of them. So, if it’s been a long time since your last dental cleaning, be sure to schedule a visit with your dentist and hygienist. Calcified plaque (tartar) can’t be cleaned off with a toothbrush and floss. It will sit there harboring biofilm until it’s professionally removed. If you see tartar buildup on your teeth or the swelling is moderate to severe, there’s likely heavy buildup under your gum tissues that needs to be cleaned off by your dental team. Do NOT attempt to do it yourself!
Overcoming Swollen Gums
Swollen gums are one of the first signs of gingivitis. If you don’t treat them, the condition can evolve into periodontal disease and tooth loss. Having a great oral hygiene plan is the best treatment and preventative strategy. But if your gums aren’t improving or you see heavy tartar buildup, be sure to schedule a cleaning with your dentist!
Make your inbox smile!
Subscribe