Warning Signs of Sleep Apnea & What To Do About It

Sleeping disorders often go undiagnosed until the symptoms are extremely severe. Unfortunately, untreated sleep apnea can seriously raise your risk of a major cardiovascular event or even death. Understanding what causes sleep apnea and what you can do to help manage your health condition is important for you and your family.
Recognizing the symptoms of sleep apnea will help you know when to reach out for help, where to go for treatment, and understand the best way to enjoy a healthier, happier lifestyle in the years ahead. And believe it or not, you can even get help for certain types of sleep apnea from your dental team!
3 Types Of Sleep Apnea
A sleep study can help you know which specific type of sleeping disorder you have, as the symptoms and side effects often overlap one another. The great news is that nowadays you can actually have a sleep study conducted at home, so you don’t necessarily need to stay in a medical lab overnight.
If you think you have sleep apnea, here are the three types of the disorder that you’ll want to be familiar with:
1. Obstructive Sleep Apnea
2. Central Sleep Apnea
3. Complex Sleep Apnea Syndrome
Warning Signs & Common Symptoms for Sleep Apnea
Not everyone experiences the same symptoms of sleep apnea. Only one or two red flags may be all you need to make the connection that something is wrong with your sleep health. Some of the most common signs and symptoms for sleep apnea include conditions like:
- Fatigue
- Frequent headaches
- Morning headache
- Difficulty concentrating
- Poor sleep
- Depression
- Weight gain
- Alcohol use
- Flat, worn teeth and broken dental restorations
- TMJ pain or disorder
- Loud snoring
- Sore throat
- Pauses in breathing while you sleep
- Waking up feeling tired
- High blood pressure
- Excessive daytime sleepiness
- Inflammation
- Falling asleep during the day
- Diminished sex drive
- Mood swings
One of the most common misconceptions about people with sleep apnea symptoms is that people with a sleeping disorder will almost always snore at night. But that’s not necessarily true. Plenty of people who snore do not have a clinical sleeping disorder, and not everyone with sleep apnea will snore when they go to bed at night.
The only way to know for certain if you have sleep apnea is to talk to your dentist or PCP about having a home sleep study or overnight test conducted to analyze your breathing and sleep health.
What Causes Sleep Apnea?
What causes sleep apnea or someone to develop a sleeping disorder? While anatomical issues and weight gain can physically block off someone’s airway, central nervous system disorders can also play a role in pauses in breathing when someone sleeps. Typically, the #1 cause of sleep apnea is attributed to weight gain.
How Do I Treat Sleep Apnea?
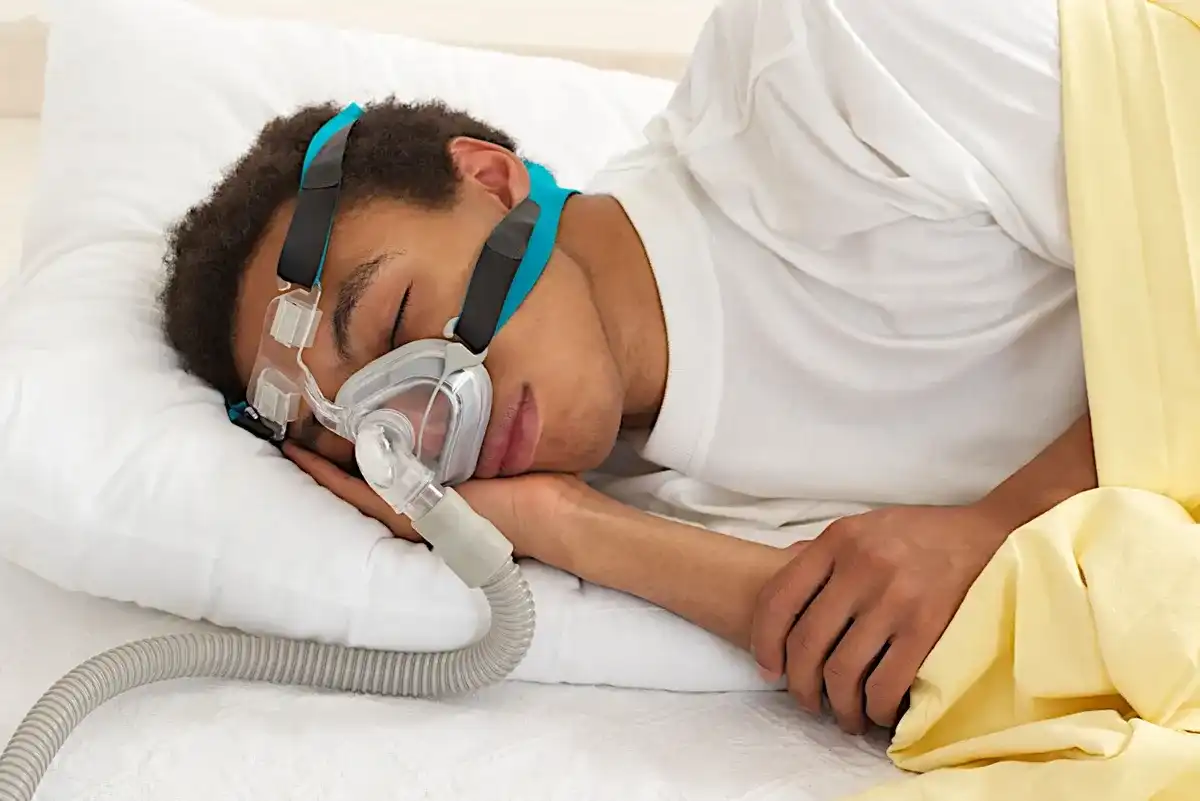
There are usually two major clinical treatment options for sleep apnea. One is using a Continuous Positive Airway Pressure (CPAP) machine and the other is a mandibular advancement device. CPAP machines physically force air into your lungs by using strong pressure delivered through a hose placed over your nose. With an oral sleep appliance, the device is fitted by a sleep dentistry provider and it positions your lower jaw (mandible) in a way that reduces the risk of airway blockage in the back of your throat. Oral appliances are FDA-approved for treating and managing symptoms of obstructive sleep apnea (OSA). However, they must be fitted by a dentist because they are technically dental appliances.
Prevention of Sleep Apnea
One of the best ways to help prevent mild sleep apnea or improve your symptoms is to get plenty of exercise and lose some weight. I know – no pressure, right? But you can also reduce your risk factors by avoiding alcohol right before bedtime since it relaxes your muscles and may put you at a greater risk of soft tissues collapsing in your upper airway.
Is Sleep Apnea Common?
Unfortunately, it’s estimated that as many as 80% of cases involving moderate to severe obstructive sleep apnea go completely undiagnosed.
Sleep Apnea FAQ
Can you die from sleep apnea?
What are the warning signs of sleep apnea?
The most common warning signs of sleep apnea are the symptoms that tend to creep up and don’t go away very easily. Like problems concentrating on a day-to-day basis, recurring headaches, high blood pressure, weight gain, tooth wear, and even changes in your mood or activity level. Snoring is not and shouldn’t be the target symptom that tells you whether or not you have a sleeping disorder. It’s just one possible symptom of dozens.
How common is sleep apnea?
Sleeping disorders are more common than what a lot of people realize. But unfortunately, not everyone seeks out medical advice or treatment. In the United States, approximately 1 in 4 adults between the ages of 30-70 have clinical sleep apnea. When you consider other types of sleeping disorders like insomnia or conditions like snoring, as many as half of us are struggling to get a good night of sleep.
Do I need a breathing machine to treat sleep apnea?
Depending on the type of sleeping disorder you have, you may or may not need a “breathing” machine or CPAP. It also depends on the severity of your condition and your compliance or ability to use certain types of equipment. For example, plenty of people can use oral sleep appliances for obstructive sleep apnea (but not central sleep apnea) without needing a CPAP machine. Or they use it in combination with their CPAP. Other times, people manage to address secondary factors, such as their weight, and improve sleep apnea symptoms by developing healthier lifestyle habits. But breathing machines are crucial for managing symptoms of more aggressive sleep-disordered breathing conditions because they physically force oxygen into your lungs. Some people cannot survive without them.
Are there home remedies that help with sleep apnea?
Actual clinical sleeping disorders need to be treated by your physician or sleep dentistry team. Most prescription devices are for use at home, such as CPAP machines or mandibular advancement aids. But it’s best to not try to buy an over-the-counter snore mouthpiece or nasal strips and hope that they do the trick. Because even though those types of devices might help with the occasional snoring or nasal obstruction, they are not effective enough for sleep apnea snores or managing a clinical obstructive or nervous-system based medical disorder.
What are the risks of not treating sleep apnea?
Untreated sleep apnea can leave you feeling tired and make it too difficult to concentrate when you’re working or trying to focus on something. Unfortunately, it also puts you at a clinically higher risk of having cardiovascular disease because of all of the strain on your body. Simply trying to get through the day is hard without any quality rest to “recharge” yourself. And then there are the more physically noticeable side-effects:
- excessive daytime sleepiness
- weight gain
- airway pressure
- high blood pressure
- saggy bags under your eyes
- worn tooth enamel from clenching your teeth all night long.
Even if sleep apnea doesn’t send you spiraling into a heart attack, your body will still take a toll from not getting the rest it needs.
Should I talk to a dentist or physician (or even a sleep specialist?)
If you’re experiencing symptoms of sleep apnea, definitely make plans to talk to a healthcare provider. For people who have flat teeth and jaw pain, be sure to chat with your dentist during your routine checkup. They can screen you for signs of obstructive sleep apnea and help you determine if you need a home sleep study. Some dental offices even offer take-home tests and oral appliance therapy with their dentist.
On the other hand, if you suspect central sleep apnea or any other type of sleep apnea, you can also get a referral from your PCP to visit a pulmonologist or sleep medicine practice. They’ll have you come in for an appointment, review your health history, and either send you home with a take-home study kit or arrange for you to take a test in their overnight lab.
Bottom line don’t wait to get help. Untreated sleep apnea could wind up putting you at an extremely higher risk of a heart attack or stroke.
Sleep Apnea Recap
For people with sleep apnea, it’s easy to overlook the symptoms if you’re used to struggling with them every day. But sleeping disorders can come with serious risk factors for your health (and life.) Understanding what causes sleep apnea and knowing when to take action can help improve your overall wellness, quality of life, and ultimately your life expectancy. Working with a sleep dentistry team or a sleep specialist can help you get a firm diagnosis on which type of sleep apnea you have so that you can take steps to address it before it’s too late. If you’re exhibiting any of the warning signs—even if it’s just one or two of them—talk to your physician or dentist about getting tested. It’s easier than you think it is, especially with the take-home tests that are available nowadays.
Make your inbox smile!
Subscribe