When Can I Stop Worrying About a Dry Socket

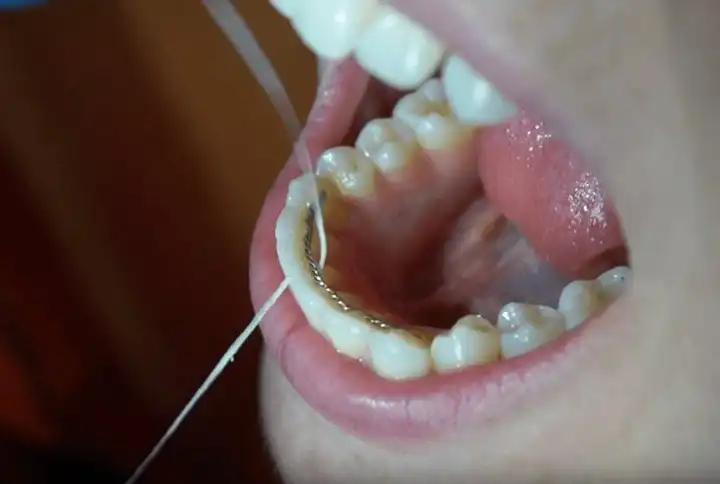
A dry socket is one of the most painful complications that can happen after a tooth extraction or wisdom tooth removal. If you’re taking steps to help prevent one, you’ll probably find yourself asking, “How long do I have to worry about a dry socket?” Once you’re in the clear, you can typically go back to your normal, everyday routine without having to worry about unwanted side effects.
Dry Sockets After An Extraction
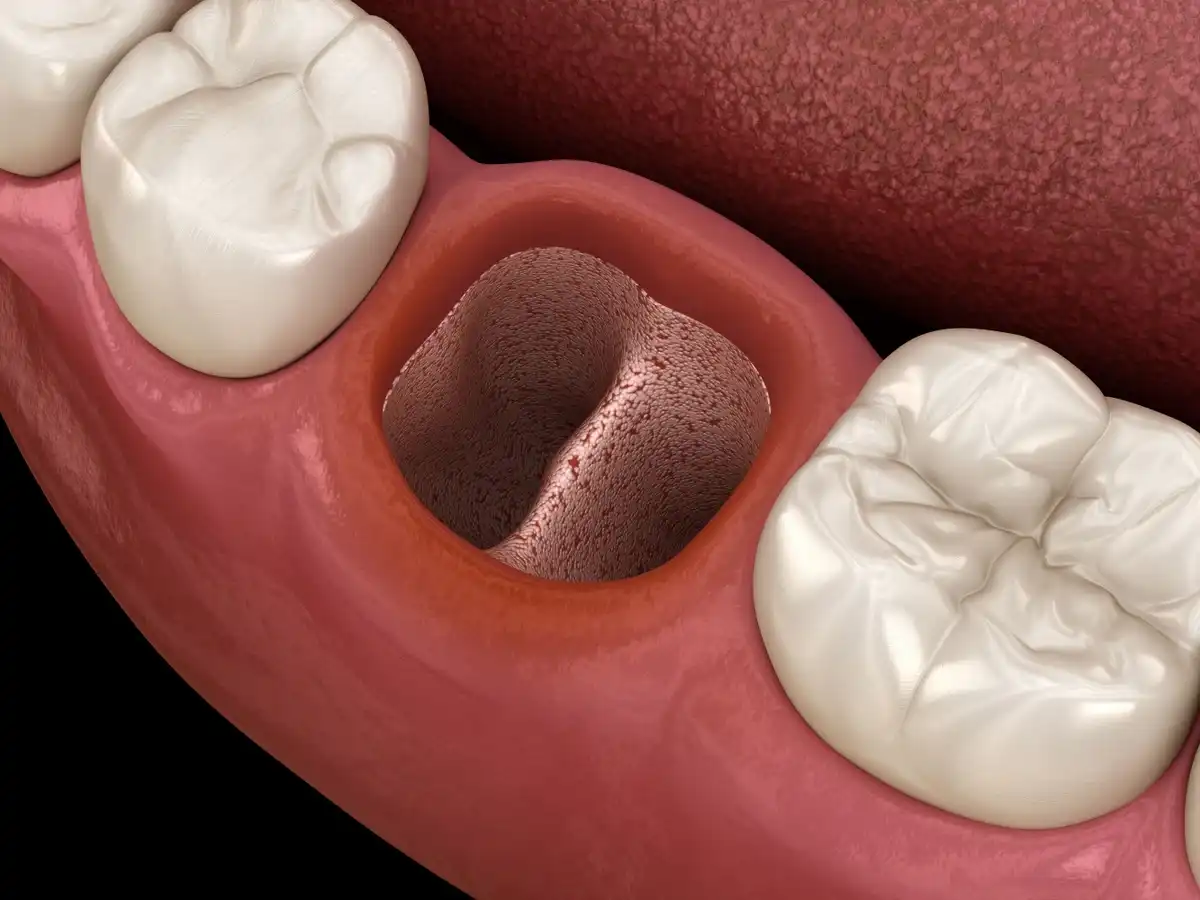
However, whenever that blood clot is disrupted and comes out of your socket, it leaves a “dry socket” in its place.
Dry sockets are extremely painful. While a typical tooth extraction can easily be managed with over-the-counter pain relievers, dry sockets typically require prescription medication to provide relief. They significantly delay your healing process by as much as 1-2 weeks, requiring that you take additional time off from work or school. These painful infections are practically impossible to power your way through. That’s why it’s important they be prevented altogether. Understanding when you’re “in the clear” will prevent you from having to worry about a dry socket after you’ve had a tooth pulled.
When Can I Stop Worrying About Dry Socket?
Normally you can stop worrying about a dry socket about 3-4 days after your dental extraction. The most “susceptible” days—if you want to call them that—are immediately after having your tooth removed. Your body will form a blood clot on the same day as your tooth extraction, or at least it should.
After about three days, most people tend to see an improvement in any tenderness around their extraction site. However, the healing process will continue for the next 1-2 weeks.
If you’ve made it 3-4 days after your tooth extraction without developing a dry socket, you are probably in the clear. But you still need to be gentle with that area because certain things like eating hard, crunchy foods, or poking it with a toothbrush could delay your healing and set you back a few days.
What Causes A Dry Socket
A dry socket happens when the tissues filling in your tooth extraction site are disrupted. Maybe they get knocked loose, physically irritated, or don’t “take” for some reason. When that happens, the blood clot comes out and the exposed bony socket is left behind.
There are several reasons why someone could get a dry socket. Here are some of the most common offenders:
Smoking
Smoking significantly dries out the mouth and delays healing because of how it causes atrophy in the blood vessels feeding your gum tissues around the teeth. This increases your risk of dry socket developing.
Eating hard or crunchy foods
Tough, crunchy, or hard textures can physically poke into your extraction site, dislodging the clot. Wait at least a week before you start eating harder or crunchy foods.
Drinking the wrong thing, the wrong way
Do not use a straw, as it could create suction inside of your mouth and pull at your blood clot. Along the same lines, do not drink restricted beverages (alcohol, caffeine, carbonated, etc.) as they could also interfere with healing.
Medical History
Not being truthful about your medical history. Your mouth is a part of your body. Even if you feel like something isn’t pertinent to your dental care, such as recent surgery or medication that you’re taking, your dentist needs to know.
Too Active
Not taking time to rest. Vigorous activity, exercise, or just not taking the time to rest could strain your body and make it difficult for your blood clot to “take” at the extraction site.
Poor Post Care
Not cleaning your mouth properly. You need to be able to safely remove food debris and bacteria to prevent infection. But if you clean around your tooth extraction site too aggressively, you have a higher risk of a self-induced dry socket. Follow your dentist’s instructions to a T.
How To Identify Dry Sockets
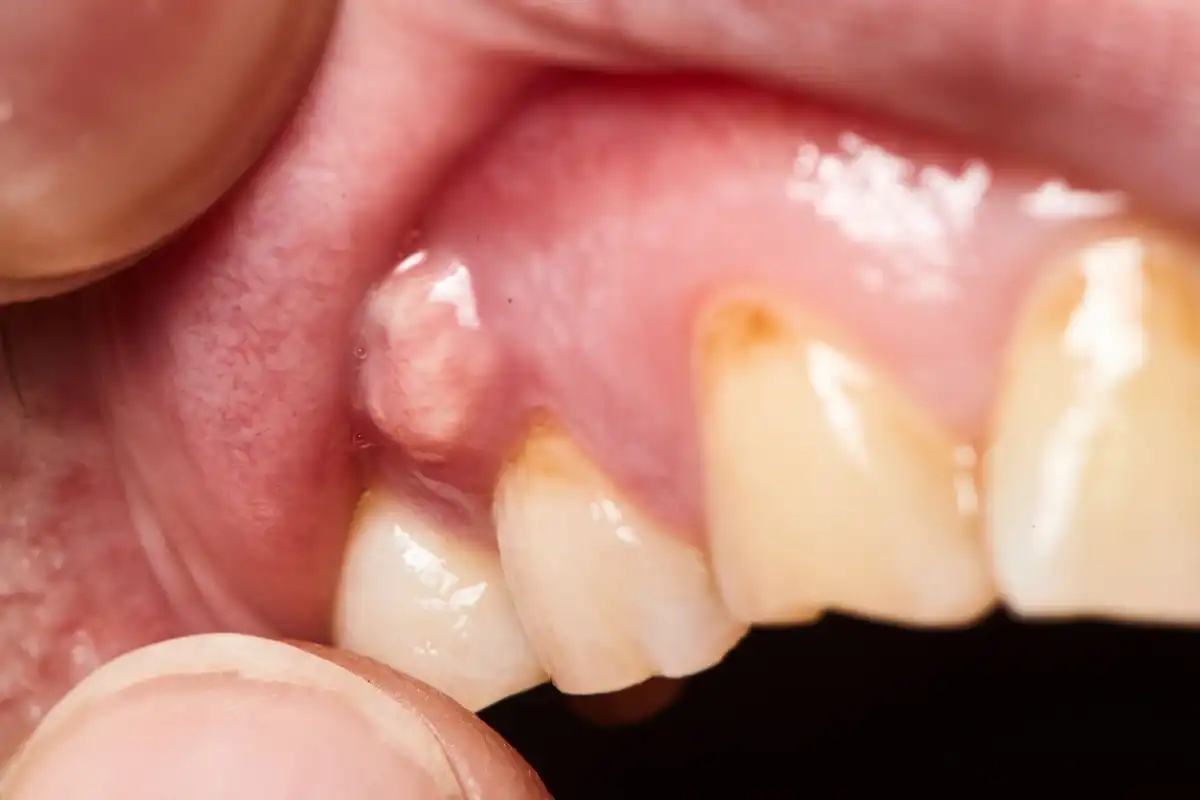
When you have a dry socket, it’s pretty difficult to miss. Typically, you’ll notice an increase in discomfort or flat-out pain around your extraction site. Swelling, redness, fever, and difficulty eating are common symptoms. There may also be a foul odor coming from that area of your mouth.
If you’re able to look inside your mouth (or have someone do it for you) you will see a visible opening. Technically there should be a blood clot covering the socket. If it isn’t and you can see down inside of the socket or visible bone, you have a dry socket.
Even if you only suspect a dry socket or your symptoms worsen 3-4 days after your tooth extraction, you need to see your dentist. They will visually assess your extraction site to confirm whether or not you have a dry socket so that you can get the correct form of treatment.
How to Treat Dry Sockets
The best thing to do if you’re at risk of a dry socket is to take steps to prevent it. But sometimes dry sockets happen anyway, even if you’ve done everything possible to protect your mouth.

To treat a dry socket, you need to start with a call to your dentist’s office. They will probably ask you to come in for an appointment so that the dentist can examine the extraction site and check that everything is ok. Depending on if there are any infections, bone chips, or sutures, they’ll decide what to do next.
First, your dentist will put numbing medication around the dry socket to get you comfortable. Then they’ll clean the area out to eliminate any bacteria that are contributing to infection or pain. Most dentists will also pack a medication down inside of the dry socket, to help jump-start the recovery process. They might even prescribe an antibiotic and pain reliever for you to take over the next week, as the area heals naturally.
Time and professional care are the best treatment. Do not attempt to treat your dry socket at home by yourself, as it could lead to serious infection, additional side effects, and significantly delay the healing process.
Dry Socket Prevention
The best treatment for dry sockets is to prevent them from happening in the first place. More than likely, your dentist provided you with verbal and/or written instructions about how to take care of your mouth for the next several days. Make. Sure. You. Follow. Every. Single. One. Of. These. Instructions. If you don’t, you’re setting yourself up for a dry socket by not taking all of those extra precautions.
This is not a comprehensive list by any means, but here are some of the things you need to do to prevent a dry socket after an extraction:
- Do not use tobacco products under any circumstances
- Do not use a straw
- Do not drink caffeinated, alcoholic, or carbonated beverages
- Gently rinse/swish with lukewarm salt water every few hours
- Avoid brushing the extraction site for at least several days
- Take all medications as directed and only under the direction of your dentist and/or physician. Do not stop using them or add to them, unless your dentist/doctor tells you to.
- Avoid vigorous exercise for about a week
- Keep required post-op appointments as scheduled
Talk to a Dentist
If you think you have a dry socket, let your dentist know immediately. The earlier they intervene, the less discomfort you’ll have to experience. More than likely, they can place medication in that area to improve your symptoms within a day.
Talk to your dentist before and on the day of your planned extraction to discuss any questions you have. The better you understand the “why” and “how” of what’s happening as your mouth recovers, the less likely you’ll be to experience a dry socket when you head home.
So, When Can You Stop Worrying About A Dry Socket
There’s always a small chance of getting a dry socket any time you have a tooth extracted or planned wisdom tooth removal. Fortunately, you don’t have to worry for very long about getting a dry socket. Your “window” is generally within the first few days immediately after the extraction. Once you make it to day four or five, your blood clot is probably in the clear. But if you don’t follow your home care instructions or start to experience severe pain in the next couple of days after having your tooth pulled, let your dentist know immediately. They can medicate your dry socket to relieve symptoms and get you on the fast track to recovery.
Make your inbox smile!
Subscribe