7 Reasons Why Your Teeth Hurt When Eating Sweets Or Sugar


Does it ever feel like your tooth hurts when eating sweets? It’s probably not the “sweet tooth” you had in mind. Whenever we see teeth sensitivity to sweets or semi-sweet food, it’s usually an automatic red flag for your dentist.
Why Are Your Teeth Sensitive To Sugar Or Sweets?
Teeth sensitivity to sweets or sugary foods almost always means there’s a cavity. If there isn’t tooth decay and your tooth hurts when eating sweets, there are a half dozen other things it might be.
Sweet sensitivity tends to be isolated. If you eat sweets or drink something with sugar in it—or even an artificial sweetener—the sweet flavor can send a jolting pain right through your affected tooth.
7 Causes of Teeth Sensitivity to Sugar
Why is it that some teeth are sensitive to sweets and sugary foods but not other things like hot temperatures, crunchy textures, or changes in the temperature?
If you’ve started noticing a sweet tooth that aches every time you drink your peppermint latte, sip on diet soda, or sneak a piece of candy, take note. Rarely does sweet sensitivity go away on its own. In fact, I’d say I’ve never seen it happen. That’s because most of the reasons behind sweet sensitivity are caused by some type of oral health condition or infection.
As you start down the path of self-diagnosing your toothaches or “sweet tooth” pain, take special note of the following common causes of sensitive teeth:
1. Tooth Enamel Erosion
Acids, bacteria, and aggressive tooth brushing can wear right through your tooth enamel. Tooth enamel erosion tends to look glossy or shiny and feel smooth to the touch. Sometimes they even look more transparent because of the tooth enamel thinning out.
Enamel erosion can also be linked to acid reflux disease or eating disorders like bulimia nervosa.
When the enamel on our teeth starts to erode, it wears out the protective cover that safeguards our smile against tooth sensitivity. Teeth that have begun eroding tend to be more sensitive than those with normal enamel.
Treatment:
With enamel erosion, there isn’t a lot you can do to treat the tooth because tooth enamel can’t grow back. But you can prevent further erosion and protect what’s there, usually by applying fluoride routinely. Severely eroded teeth may need protective covers like crowns or veneers to help them look healthy and whole again. Especially if the enamel is starting to chip away or your teeth are extremely sensitive.
2. Tooth Decay
There’s about a 9 out of 10 chance that your tooth hurts when eating sweets because you have a cavity. Sweet sensitivity is just one of those things that go hand-in-hand with tooth decay. It has to do with the way sweet foods or drinks irritate the nerve tissues inside of your tooth.
Treatment:
The only treatment for a cavity is to remove the decayed portion of your tooth, clean that area out, and place a filling inside of the void. Fillings help prevent the spread of decay, which is actually a bacterial infection. Untreated cavities will expand deeper into the tooth and eventually reach the nerve; by that point, a root canal and crown are the only treatment options left.
3. Gingivitis
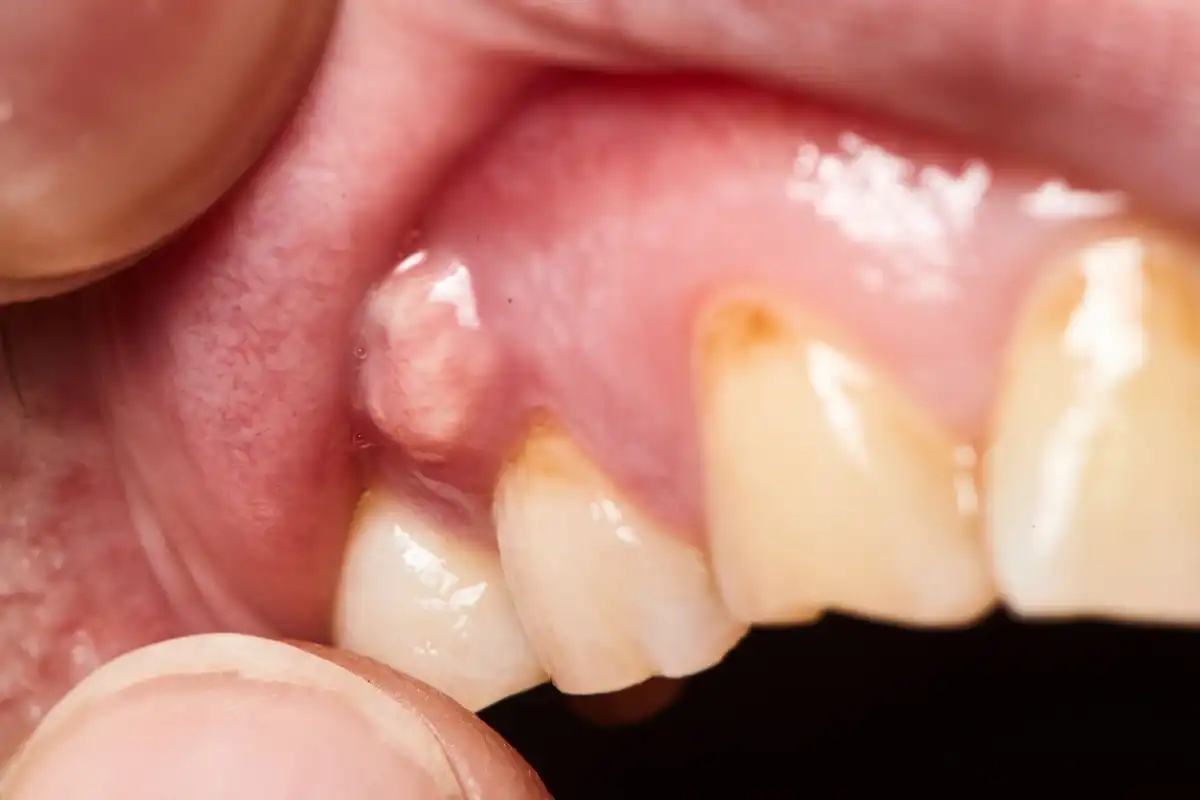
When your gums are swollen, red, or bleed, it’s usually because of gingivitis. Gingivitis can make your teeth and gums feel more sensitive than normal, especially when something like a toothbrush touches them. There’s probably a red area on your gums closest to the tooth if it’s gingivitis.
Gingivitis needs to be treated in a timely manner so that it doesn’t evolve into a more aggressive gum disease. While gingivitis is totally reversible, gum disease or periodontitis isn’t. By the time you start seeing gum recession, gaps between teeth, tartar buildup, and loose teeth, a periodontal infection is probably present.
Treatment:
The best treatment for gingivitis is improved daily oral hygiene. Brushing twice a day and flossing every day will typically reverse gingivitis symptoms within a couple of weeks at the most. Gingivitis and periodontal disease can be treated with deep cleanings. If areas of inflammation or bleeding don’t improve by that point, your dentist will probably need to check for gum disease.
4. Receding Gums
Your gum tissues (gingiva) are a protective cover for your tooth roots. Roots, unlike the top of your teeth, don’t have a hard enamel layer covering them. When the gums pull back and expose your tooth roots, the tiny nerves inside of the porous tooth surfaces tend to be extremely sensitive, if not painful.
Common symptoms of gum recession are visible tooth roots, spaces between teeth, tooth sensitivity, and tooth mobility. Some people just tend to call it “long in the teeth.” But gum recession isn’t just about getting older. If your dentist or hygienist performs a periodontal screening, there will be measurable areas of gum detachment and/or “pocketing” around affected teeth if you have an infection.
Treatment:
Treatment for receding gums starts with addressing the cause of your receding gumlines. Are you brushing too hard? Do you have gum disease? Is a tooth out of alignment, causing the gingiva to pull away? Depending on your situation, your dental team will create a care plan that could range from deep cleaning to orthodontic therapy.
Moderate to severe gum recession might also require a gum “graft.” That’s where gum tissue is moved over your exposed tooth to re-cover it and protect the sensitive root underneath.
5. Poor Oral Health
If you don’t have great oral hygiene, you probably have heavy plaque buildup along your gums, visible tartar buildup here and there, and red or swollen gums that bleed easily. Because poor oral hygiene allows a sticky film called plaque to sit on your teeth for long periods of time, the bacteria will slowly etch away at your teeth and cause cavities. The problem is you might not see the decay because it’s covered up by thick layers of plaque.
Using a disclosing agent can help dye the plaque pink or purple, helping you see where it’s the heaviest. Depending on how long the buildup has been there, plaque deposits will vary in color from light pink to dark magenta or purple.
Treatment:
This one is easy. It’s time to re-vamp your oral hygiene routine. Start by brushing for a minimum of two minutes twice a day. If possible, get an electric toothbrush. Make sure you’re cleaning the outside, inside, and chewing surface of every tooth, especially right next to the gums.
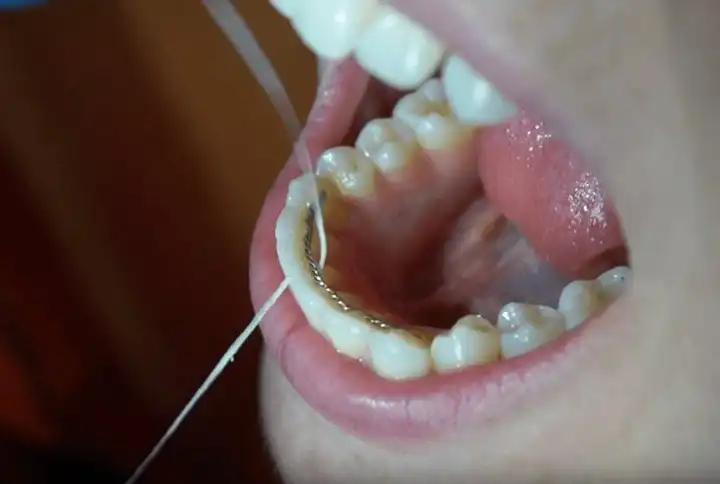
Next, make sure you’re flossing the right way. Once a day is key. Wrap the floss in a “C” against your tooth and rub it up and down a few times, then move to the next tooth. Be sure to have the floss slip just below your gumlines, too.
6. Medications
If you’re taking medication that dries out your mouth, you’ll be more likely to develop new areas of decay and tooth sensitivity. Your saliva acts like a natural buffer against bacteria, food, and the outside environment. But dry mouth leaves teeth exposed to bacteria and sugars.
Unfortunately, dry mouth is one of the most common side effects to see on the label of just about any medication, whether it’s prescription or over the counter. Decongestants and antihistamines, especially. There are actually over 400 drugs that list xerostomia (dry mouth) as a side effect when you take them.
Treatment
If you have to take a medication that causes dry mouth, make sure you’re drinking plenty of water, brushing daily, limiting your sugar intake, and flossing every day. It’s also helpful to add fluoride gel or rinse into your daily oral hygiene routine.
Sugar-free gums or mints can help with saliva production. Personally, I recommend gum that has xylitol in it because it helps prevent bacteria from sticking to teeth, ultimately lowering your risk of cavities or sweet sensitivity.
7. Tooth-Whitening Treatments
Whenever you apply a whitening agent to your teeth, it opens up the tiny micro-pores called “tubules” across the surface of your tooth enamel. Almost all tooth whiteners contain hydrogen peroxide which penetrates the teeth' top layer and tubules, increasing tooth sensitivity. This can make some people have more tooth sensitivity than normal. And if you’re whitening in an area of your mouth where there’s gum recession, the root surface is likely to be hypersensitive after the gel is applied. Usually, the sensitivity tends to develop after the first few applications and is triggered by eating something cold (or, in this case, sweet.)
Treatment
Always communicate your tooth sensitivity with your dentist. They may recommend tooth whitening treatments with weaker concentrations or different types of whitening gel than other people use. Another thing you can try is alternating which days you whiten instead of wearing your kit every single day in a row.
Using a sensitive tooth toothpaste and/or fluoride leading up to your whitening treatment, during the process, and for a couple of weeks afterward, will help prevent whitening-induced tooth sensitivity.
Related: Best Sensitivity Toothpastes
Preventing Teeth Sensitivity to Sugar
- Eat dessert right after your meal to limit acid exposure time on teeth.
- Only drink water between meals.
- Avoid sticky textures that will cling onto your teeth for hours afterward.
- Use a straw for drinking, especially if it’s something like carbonated soft drinks or sweet tea.
- Limit liquid sugar intake, including artificially sweetened drinks.
- Floss around and between every tooth, every day.
- Brush twice a day, paying particular attention to the areas closest to your gums with a soft-bristled toothbrush.
- Consider using toothpaste designed for sensitive teeth.
- Rinse with a fluoride mouth rinse after brushing and flossing.
- Schedule regular checkups and cleanings every six months.
- Have cavities treated quickly, before they have a chance to spread deeper into your tooth.
Once sweet sensitivity starts to flare up, you usually can’t get rid of it on your own without the help of your dentist. Especially if it’s because of enamel erosion, gum recession, or active decay.
Related: Best Electric Toothbrushes for Sensitive Teeth and Gums
Candy & Sweets to Avoid
If you have an issue with sweets, teeth may be more sensitive to some sources of sugar than others, such as hard or sticky snacks that get stuck in your teeth or acidic drinks with a low pH level. Even if you have mild gum recession, some foods are more irritating to your teeth.
What are the worst candies and sweets that cause cavities? Are some worse than others? Actually, yes. If you’re prone to sensitive teeth, tooth decay or trying to do your best to avoid issues altogether, here are some things you’ll want to avoid on a day-to-day basis:
1. Hard Candies
Hard candy is something you tend to suck on for several minutes at a time. And chances are, you probably don’t have just one piece. Every time you consume sugar, it exposes you to about 30 minutes of acid in your mouth afterward.
2. Gummy Candy
Anything that can get stuck to your teeth has the potential to stay there for hours, releasing sugar in your mouth. Caramel, fruit chews, and bubble gum or any other gummy or sticky sweets never a good idea.
3. Fermentable Carbs
Processed and fermentable carbohydrates (like white flour or starchy food) feed the bacteria in your mouth that secrete cavity-causing acids whenever you eat them!
4. Sugary Drinks
Yes, soda contains sugar. But so do sports drinks, energy drinks, coffee creamer, diet sodas, and fruit juice. Be careful; liquids get in all of those nooks and crannies, which is why they’re so bad about causing cavities.
5. Orange Juice
Acidic fruits can really do a number on some people’s teeth. Orange juice and other citrus products could cause sensitivity, especially if you have gum recession or enamel erosion.
Talk With Your Dentist
Any time a tooth hurts or is sensitive, you need to make a mental note of it. If it happens more than once or twice, it’s time to call your dentist. Especially when it comes to sweet sensitivity or isolated tooth pain. It’s better to err on the side of caution and address an issue like minor gum recession than it is to accidentally ignore a warning sign of tooth decay. The earlier dental issues are addressed, the more conservative and affordable your treatment options are. Being on top of the issues can keep your teeth healthy in long run. You might only need some fluoride or a little dental bonding, as opposed to a crown or root canal.
So, Why Do My Teeth Hurt When I Eat Sweets
Whenever someone says their tooth hurts when eating sweets, I instinctively want to check the tooth to see if signs of tooth decay are present. Usually, teeth sensitivity to sweets means a cavity. But sometimes it’s enamel erosion, gum recession, or an issue related to poor oral hygiene. Plan for the worst and hope for the best. You can always try a sensitive toothpaste or fluoride to see if your symptoms improve. Then call your dentist if you feel the pain or irritation more than a couple of times because it’s better to be safe than sorry.
Make your inbox smile!
Subscribe