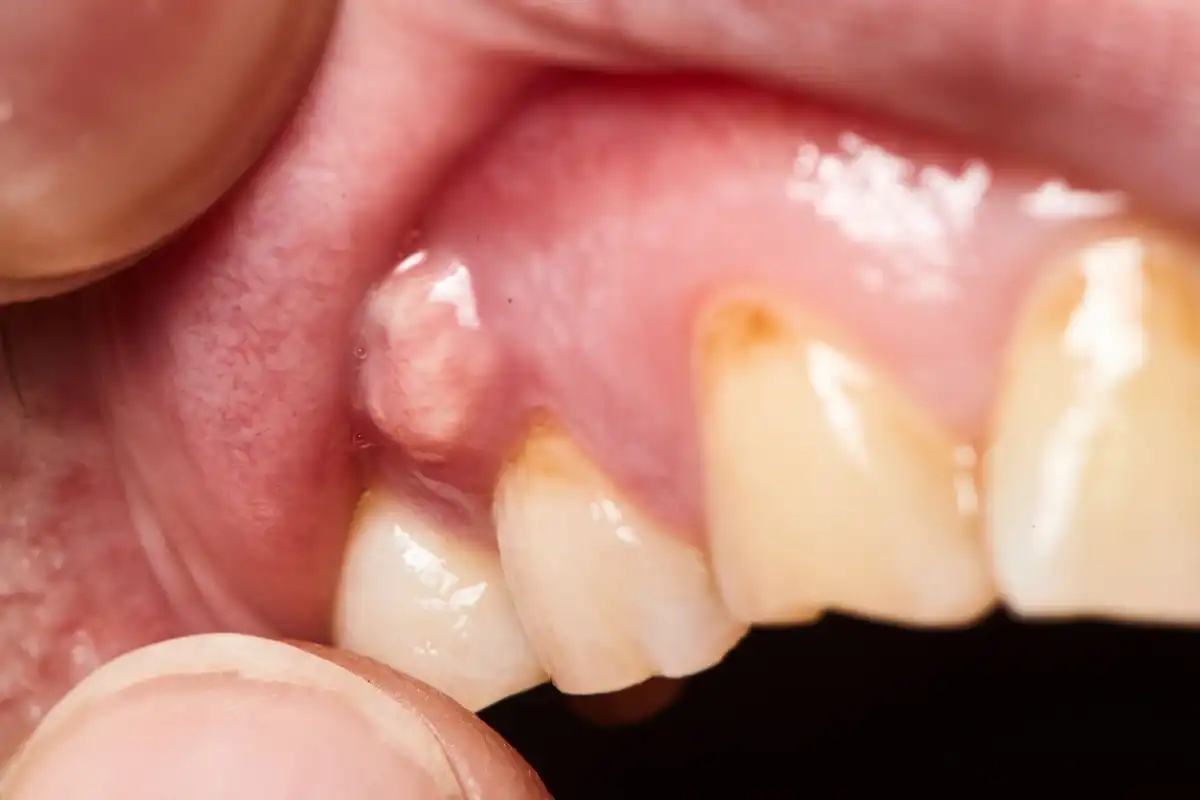
13 Reasons Why You Have a Bump on the Roof of Your Mouth

Your mouth is extremely sensitive. Even the tiniest changes are often picked up by your tongue. Small chips, a bump on the roof of your mouth, or even a tiny ulcer under your tongue are easy to pick out from the healthy or “normal” oral tissues around them. And as with other places on your body, any time you feel a nodule, swelling, or bump (on the roof of the mouth, for instance) it can be a cause for alarm. A quick self-assessment and diagnosis can help you figure out if the growth is something you need to be concerned about.
The roof of the mouth is made up of two parts: a “hard palate” (the firmer texture toward the front of your mouth) and a “soft palate” (softer area toward the back of your throat and tonsils.) Depending on where the sore or bump is in the roof of your mouth, symptoms could indicate varying different medical diagnoses.
Should I Be Concerned?
Any time you suddenly feel a growth or bump on the roof of your mouth (palate) or the areas around it, it should catch your attention. Typically, these sorts of anomalies do not occur overnight. The roof of the mouth is a hard bony structure that is covered by a dense layer of mucosa (tissue), making it far less likely to be prone to swelling or bumps. This reason alone is enough to raise the sound for alarm if you notice a growth or swelling across your palate behind your teeth.
Causes For A Bump On The Roof Of The Mouth
Our bodies naturally swell or bruise if we bump into something too hard. But our mouth — and in this case, our palate — typically doesn’t work that way. Yes, you may see swelling if you bite down on your cheek accidentally, but it’s far less common for a traumatic injury to cause a bump on the roof of mouth/palate. If you do see swelling in your palate, you’ll want to rule out these common causes:
1) Canker Sores
Canker sores (also called aphthous ulcers or just plain ol’ “ulcers”) are temporary sores that can form anywhere in your mouth. Canker sores tend to be extremely tender, flat, raw-looking or white as they start to heal, or have a slight sunken-in surface. If inflamed, they may appear raised instead of crater-like. It’s not very common to see canker sores on the roof of the mouth, as they tend to pop up in areas like the lips and cheeks more frequently. Most of the time canker sores are because of irritation to a specific part of your mouth – like braces rubbing your cheek – or because of stress/illness/etc. Canker sores tend to make eating and drinking uncomfortable for the first few days after they flare up.
Treatment
The best treatment for a canker sore is being gentle to it and giving your mouth some time to rest. Avoid hard or crunchy foods, such as pretzels or tortilla chips. Additionally, acidic foods should be avoided as they tend to irritate the raw ulcerations. Make it a goal to just keep your mouth as clean as possible without physically irritating the ulcer itself. Regular warm saltwater rinses throughout the day are helpful. Apply topical numbing products as needed and stick to a soft diet for several days. If you wear removable appliances such as an orthodontic retainer, have it evaluated for any irritating edges that need to be smoothed off (do not, I repeat, do not try to smooth out any of your dental appliances at home.)
2) Burns
Your palate is one of the most common places inside of your mouth to get burned by food. Just think about it. Any time you bite into something that’s too hot — particularly pizza or something else with melted cheese — it immediately starts to burn the roof of your mouth. By the time you get it out of your mouth, it’s already been there for a couple of seconds. These soft tissue burns tend to occur closer to the front of your palate and last for several days, causing pain every time you eat or run your tongue across them. You’ll probably notice some tissue sloughing off as the area begins to heal.
Treatment
Most oral burns just need time to heal. Avoid eating any other hot foods in the meantime (or hot cups of coffee.) Try to choose soft foods, the cooler the better, that won’t irritate your mouth as much when you’re swallowing. In the meantime, you can ease discomfort by taking an anti-inflammatory such as Motrin as needed. If the burn doesn’t heal, ask your dentist to check it for signs of infection. And in the future, always be sure to check the temperature of your food before taking a big bite out of it.
3) Cold Sores
“Fever blisters” and “cold sores” are a type of ulcer that’s caused by a specific strain of herpes virus. Don’t worry, this virus also causes shingles and chickenpox. But inside of your mouth it tends to lead to one large sore or a cluster of smaller pinprick-sized blisters. Most people recognize cold sores by the tingling or burning sensation that’s evident a day or two prior to the ulcer forming. Then blisters start to pop up on your lips or oral mucosa. After the blisters rupture, a large crater-like lesion will become evident and slowly start to crust over. They’re most frequently found on or around the lips, rather than in the roof of the mouth.
Treatment
Prescription medications are available for people with recurring cold sores. The key is to begin applying the ointment as soon as fever blisters symptoms being to develop. If your dentist offers laser cold sore treatment, contact them as soon as you feel the tingling pinpricks of the fever blister. Early laser treatment can cut the lifespan of a cold sore by half. And when all else fails, you can simply choose to wait it out and let the sore heal on its own. Two weeks is generally all that it takes.
4) Oral Mucocele
Treatment
Most oral mucoceles pop on their own. Severe blisters or a large bump on the roof of your mouth/palate surfaces may need professional intervention. If the blockage is due to something like a “salivary stone”, it can work its own way out or may have to be removed by your dentist or an oral surgeon. Otherwise the mucocele will typically keep popping and coming back over and over as more fluid builds up.
5) Epstein Pearls
Treatment
Epstein pearls tend to go away on their own over time. No formal treatment is required. Older children and adults will not have Epstein pearls, as the growths only affect infants. As your child sucks or nurses, the stimulation to that protrusion causes it to resorb (shrink). Since they are so small, it’s unlikely for Epstein pearls to interfere with feeding.
6) Trauma/Injury
Facial injuries typically occur from accidental falls, automobile wrecks, or athletic activities. But for an injury to form in the roof or floor of the mouth would have to come from some type of intraoral trauma. For example, maybe you're trying to remove a tonsil stone with a spoon in your mouth and someone bumps into you, causing the end of the spoon to jam back into your throat — you get the picture — when something like that happens, it can lead to a pretty serious injury. These types of traumatic injuries typically happen when you have something in your mouth and then accidentally fall down against it.
Treatment
As with normal bumps and bruises, time is the best medicine. Some swelling or bruising will be evident for several days as your body heals. But if the injury was severe enough to break the skin, cut your palate, or you’re unable to eat, you need to see someone. An oral surgeon will probably be your best bet, as they frequently have more resources to repair oral injuries outside of broken or knocked out teeth. If the injury is minor and no sutures are needed, stick to a soft diet and give yourself some time to heal. In the meantime, be sure to rinse with warm saltwater and take an anti-inflammatory medication for pain relief.
7) Torus Palatinus
If you’ve got a prominent, hard bump on the roof of your mouth, there’s a really good chance that it’s something we call “palatal tori” or torus palatinus if you want to sound scientific! Tori are bony protrusions that grow from your palate in the midline of the roof of your mouth.
Palatal tori usually won’t cause any pain. However, their inconvenient size and location can make them easy to irritate during everyday activities (which may make your mouth sore.) Additionally, large tori can interfere with wearing a denture.
Most areas of tori will continue to grow larger each year. Some are smooth and flat while others are quite bulbous. Depending on how large and “lumpy” it is, it may be impossible to clean underneath the tori with anything other than a water flosser. Tori can be small or so large that they cover almost the entire roof of your mouth.
NOTE: you can also get a similar growth called exostoses along the floor of your mouth or outside of your jaws, near the roots of your teeth.
Treatment
The only treatment for torus palatinus is surgical removal. Most people will only have their tori taken out if they’re planning to get a denture or the growth interferes with speech/eating. Unfortunately, there’s some bad news. Tori tend to want to grow back after you have them removed. If the surgery is so that you can wear a “plate” style denture that fits across the roof of your mouth, you may be out of luck.
8) Oral Cancer
Treatment
The best “treatment” for oral cancer is to get screened routinely so that cancerous tissues can be spotted in their earliest stages of development. After a positive biopsy result, you will work with an oncologist and possibly an oral surgeon to remove the cancerous growth and take the next applicable steps in your care plan. Do not wait until the cancerous area hurts; by then it may be too late.
Less Common Causes
1) Yeast Infection/Candidiasis
Treatment
Begin by cleaning your denture as prescribed and removing it at night, so that your mouth has time to rest. Clean your mouth daily with a soft washcloth and lukewarm water. Your dentist will likely prescribe an anti-fungal medication to take until the initial symptoms resolve. However, yeast infections can recur if the bacteria are not controlled (or your denture and mouth aren’t cleaned properly.) Good oral hygiene is essential, as thrush thrives on bad bacteria. If your doctor puts you on an anti-fungal medication, they may also suggest upping your intake of probiotics and yogurts, to aid in healthy bacterial colonies.
2) Coxsackievirus (Hand Foot And Mouth Disease)
Treatment
If you have mouth sores from hand, foot, and mouth disease, your dentist can prescribe a numbing mouth rinse to help you eat and drink comfortably. Otherwise the most common treatment is to simply allow the coxsackievirus to run its course (just like you would with chicken pox.) The average outbreak timeline is around 10 days from onset to when the sores finally go away.
3) Squamous Papilloma
Treatment
If the papillomas interfere with your appearance or make it difficult to eat, you can choose to have them surgically removed. Since the growths look similar to a wart, some people prefer to have them removed. Fortunately, they are not one of those growths that tend to come back (as long as they’re completely cut out.) Since papillomas tend to be asymptomatic, treatment usually isn’t necessary unless it’s for functional or cosmetic purposes.
4) Hyperdontia
Some people have extra teeth. These bonus teeth are referred to as “supernumerary teeth” or the person is said to have hyperdontia. Adults have 32 teeth in all, but someone with hyperdontia will have 33 or more teeth. The most common areas to see extra teeth are around the wisdom teeth (third molars) or between the top two front teeth, which is called a “mesiodens”. Hyperdontia may be due to genetics, or various types of medical syndrome. These extra teeth come in all sizes; some may be extremely small while others are the size of a fully developed adult tooth. You may not even realize that you have an extra tooth until your dentist takes an X-ray.
Treatment
Supernumerary teeth are usually left in place unless they are causing damage to the teeth around them. If they are creating pressure that moves your teeth (leading to crowding or crooked areas) or damaging the roots of the healthy teeth next to them, an extraction is usually suggested. If the extra teeth are around your third molars, they’re usually extracted at the same time of your planned wisdom tooth removal surgery.
5) Nasopalatine Duct Cyst
Treatment
Complete removal of the cyst is recommended. Depending on how large the cyst is, your oral surgeon may need to incorporate a bone graft or platelet rich plasma (PRP) therapy to help fill in the void where bone is missing.
When To See A Doctor
If you’ve ruled out a traumatic injury, given yourself plenty of time to heal, or if the sore/bump on the roof of your mouth is interfering with being able to eat, then you need to go ahead and speak to your dentist. They’ll fully examine all areas of your mouth, perform a medical screening, take any applicable X-rays, and have access to biopsy services if required. Piecing each clue together, you and your dentist can determine the cause of your swelling/sore and take steps to treat it appropriately.
Never wait more than two weeks to seek out professional care. Any sore or lump that does not resolve on its own or keeps recurring will need a formal evaluation.
Understanding A Bump On Your Palate
Occasionally it’s normal to see a bump on the roof of your mouth pop up. Other times, it’s a serious issue that requires immediate medical intervention. While typical sores like ulcers tend to heal within 10-14 days, anything that grows larger or doesn’t go away will need to be evaluated by a professional. Don’t wait more than a couple of weeks before you reach out for an exam. Fast action could be key to saving your life.
Make your inbox smile!
Subscribe