How to Treat Lingering Oral Thrush OTC & Medications

Oral thrush is technically a “yeast infection” inside your mouth. It’s also sometimes referred to as “candidiasis.” But before you get too grossed out, rest assured that you can get a yeast infection almost anywhere on your body. Especially places that are always moist or tucked behind clothing without a lot of air flow. Oral thrush is most known for affecting babies, elderly, and people who are immunocompromised or have recently been ill. Especially if they’ve been on antibiotics, which kill a lot of the natural “oral flora” (normal bacteria) found inside our mouths.
What Is Oral Thrush?
A lot of the time, we see oral thrush when there’s inadequate oral hygiene or because antibiotics are killing off a lot of different microbes in your body.
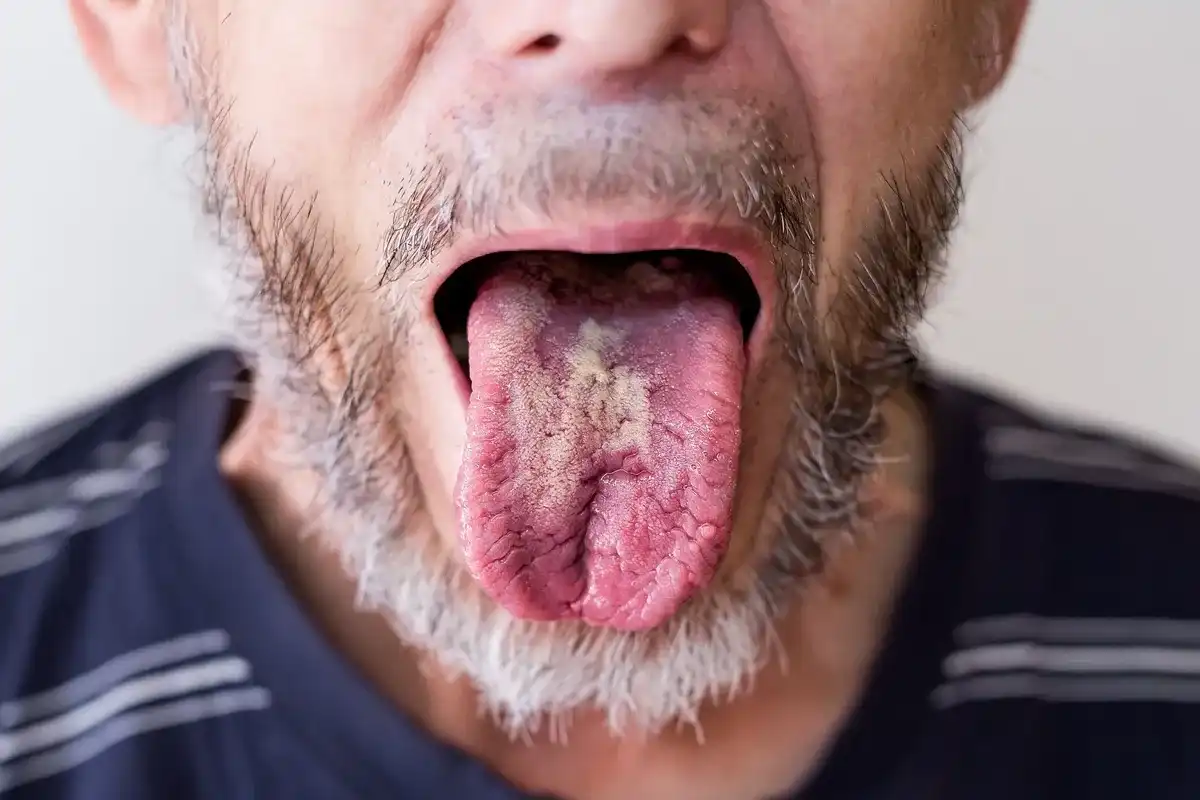
Oral thrush usually presents itself as a white, cottage-cheese like residue inside your mouth. When it’s wiped off, the skin underneath tends to be raw and bright red. It can also cause a white filmy-like appearance on the surface of the tongue. You might even have cracking at the corners of your mouth or a loss of taste.

As a yeast infection, it’s possible to see oral thrush that won’t go away in adults if there are ongoing issues at play. Such as poor home care, extended medication use, or immunodeficiencies.
Why Is Your Oral Thrush Not Going Away?
Oral thrush that won’t go away in adults is usually because of something underlying, like:
- Taking antibiotics for a long time
- Gargling with hydrogen peroxide on a regular basis
- An autoimmune disease
- Poor oral hygiene
- Diabetes
- Cancer
- HIV/AIDS
- Sleeping in your denture at night instead of removing it
If oral thrush has gotten so bad that it’s not going away within a week or so, professional medical or dental care is a must. Normally it’s best to have your dentist evaluate your mouth to make sure it’s not something else going on. From there, they can discuss how to treat oral thrush with medication and a few oral hygiene modifications. Without something to jump-start your immune system and regain control over the bacteria levels in your mouth, the oral thrush will simply keep recurring or even get worse.
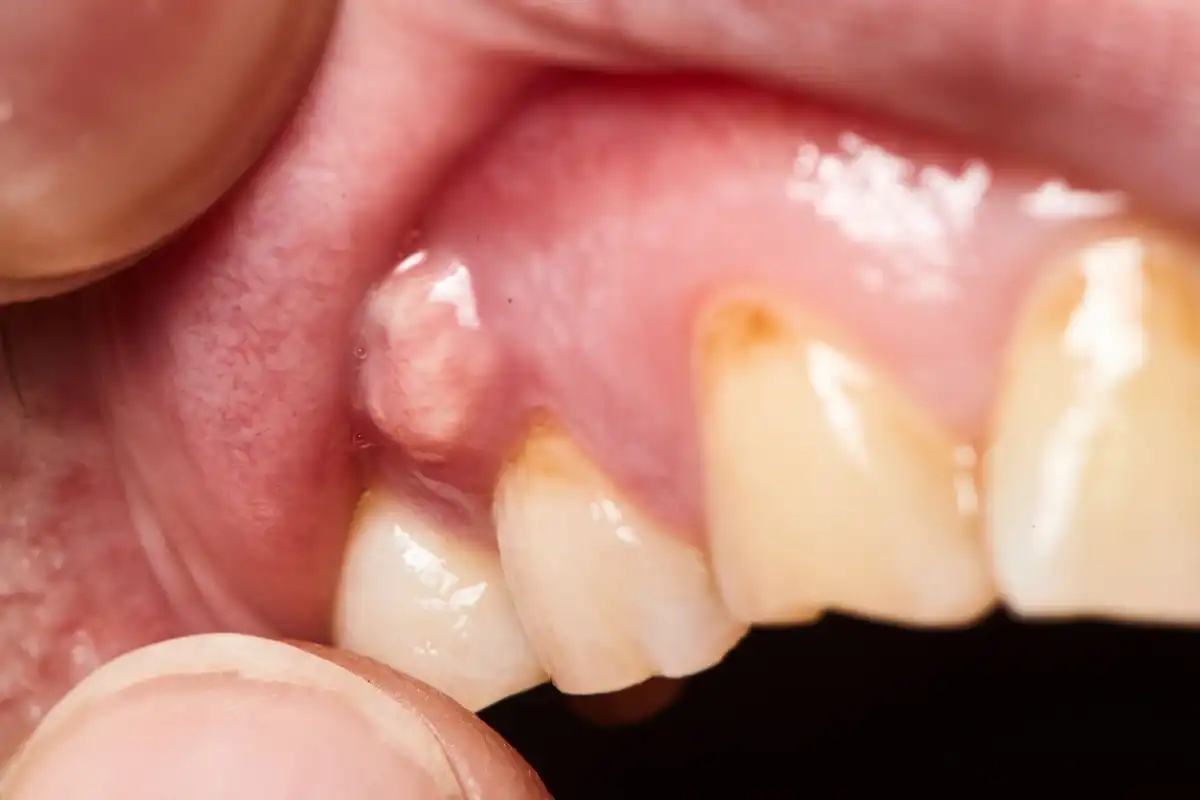
People who wear dentures can also develop an oral candidiasis infection known as “denture stomatitis” which is like thrush in the roof of their mouth.
Over The Counter Oral Thrush Treatment
Probiotics contain “good” bacteria that your mouth needs to stay healthy. By increasing certain healthy bacterial colonies, you can stabilize the ones that are out of whack, so to speak.
If you’re cleaning your mouth with hydrogen peroxide or rinsing with it, stop. It can throw off your oral flora and may make it harder to clear up a yeast infection.
For people on antibiotic therapy, make sure you’re taking your prescription as directed. If you aren’t—maybe you stop taking it because you feel better and aren’t sick anymore—it can lead to drug resistance. When that happens, you’re more likely to need more antibiotics to clear up any residual infection. It goes round and round, until you’ve had so many antibiotics that your body’s normal bacterial levels get out of control.
Oral Thrush Medications
Let’s say you’ve reached the point where you have oral thrush that won’t go away (in adults) and need to do something about it. So, you call your dentist and schedule an exam. Chances are, they will prescribe one of the following categories of medications:
Antifungals
You’re probably used to hearing about people using antifungals for athlete’s foot or needing an antifungal cream for a feminine yeast infection. Well, they’re also used for oral thrush. But only in certain forms!
Assuming your dentist confirms that you have oral thrush, they will prescribe an antifungal product such as a mouthwash, lozenge, tablet, or even a liquid. Just like other medications, you need to use it as directed in order for it to work properly. If it says to take it for 10-14 days, don’t stop using it after 5-7 days when your symptoms clear up; use it the entire length it’s prescribed.
Antifungals are the preferred treatment for oral thrush. If you want to clear up your infection quickly, this is usually the way to do it. Your dentist might even be able to work you in for an emergency appointment if the thrush is pretty bad. You could have a prescription in hand the same day.
Antiseptics
Another option is to use an antiseptic rinse or cream if you have thrush. Just keep in mind that oral yeast infections can actually be brought on by some mouth rinses, so if you aren’t careful, you might make the symptoms worse. Especially if it’s a strong antiseptic rinse that contains alcohol, which will likely cause major burning sensations inside your mouth because of your raw skin.
On the other hand, rinsing with warm saltwater can sometimes soothe oral inflammation and gently clean your mouth, even when areas feel too tender to touch.
Prescription-strength oral antiseptics are available, but most dentists prefer to use antifungals for treating thrush. Antiseptic rinses like chlorhexidine (Peridex) might be counterproductive, because of how raw and sensitive your oral tissues are.
Prescriptions For Oral Thrush
Most oral thrush prescriptions can be called into your local pharmacy and picked up the same day. Your dentist might even have some in their office. Again, these are usually prescription-grade antifungals, and most people will start to see an improvement within a couple of days.
Some of the most commonly prescribed medications for thrush include:
Mycelex (Clotrimazole)
Mycostatin (Nystatin)
Miconazole
Diflucan (Fluconazole)
Oral Thrush Prevention
What are some ways to prevent your chances of developing oral thrush?
- Always take medication as prescribed, regardless of which type of medication it is
- Change out your toothbrush a day after beginning a new antibiotic or oral thrush medication, then again about mid-way through
- Remove your dentures nightly and clean them as directed, as sleeping in a denture or partial can predispose you to getting oral thrush
- Take a probiotic or eat foods with natural probiotics inside of them if you’re about to start an antibiotic regimen
- Don’t rinse with harsh mouthwash or hydrogen peroxide
- Try not to cross-contaminate things like clean toothbrushes in dirty toothbrush holders, or clean dentures in unclean storage cases
See a Doctor
If you develop oral thrush that doesn’t get better within a few days, you need to speak with your dentist or medical doctor. And if your infection continues to recur after treatment, definitely be sure to speak to your physician. They’ll need to rule out any potential immunodeficiencies and possibly run some bloodwork if you’re prone to ongoing oral infections. Especially if you suspect an undiagnosed medical condition.
Treating Oral Thrush That Won't Go Away
Trying to figure out how to treat oral thrush? If you’re struggling with a case of oral thrush that won’t go away in adults, kids, or elderly individuals, your dentist can help. Make sure to take all of your medication as prescribed and always speak to a doctor if you’re developing recurring oral thrush, as something bigger may be at play. In the meantime, practice good oral hygiene and consider taking probiotic supplements to help.
Make your inbox smile!
Subscribe