8 Signs Of Failed Dental Bone Graft

If you’ve ever had gum disease, a severe facial injury, undergone oral surgery, or are considering dental implants, you may have gotten or need to get a bone graft. Bone grafts are routinely offered by a specialist, such as a periodontist or an oral surgeon. But grafting can also be placed in your regular dental office. The last thing you want is a failed dental bone graft. Being able to identify dental bone graft failure signs and symptoms is important!
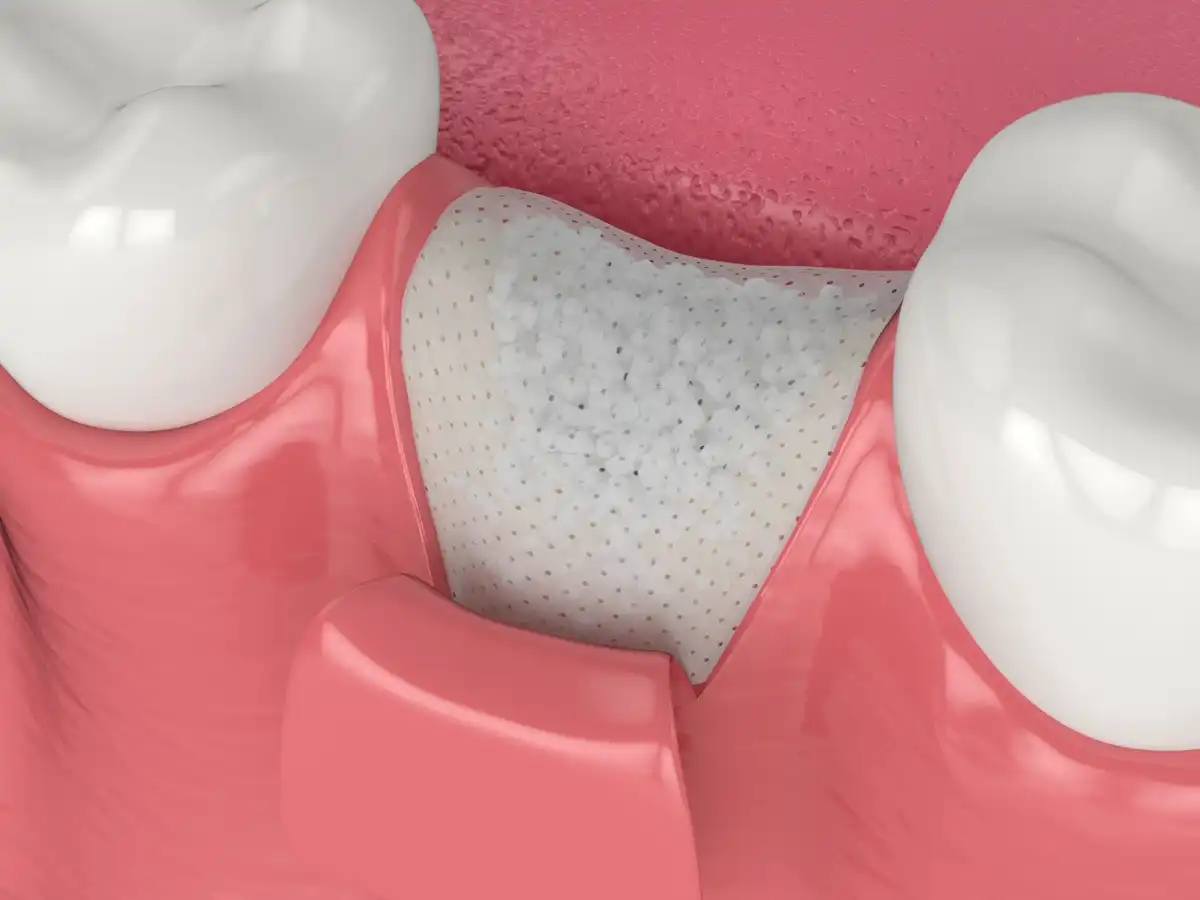
What Is a Dental Bone Graft?
A dental bone graft is where your dentist or dental specialist goes in and places bone tissue in an area where your natural bone is weak. For instance, maybe your bone shrunk because you had missing teeth and your dentist needed to strengthen that area before you could get a dental implant.
How Do I Tell If The Bone Graft Failed?
The last thing you want during smile reconstruction is a failed dental bone graft. If the augmentation (graft) site is failing, it delays your overall treatment and recovery process. For people with missing teeth, a delay can be especially challenging. If you know how to spot dental bone graft failure signs early, you can potentially limit your chances of a failed dental bone graft.
Anytime a bone graft is placed, that area of your mouth should heal the same as any other. Dental bone graft failure signs are fairly obvious in most cases because you won’t see the recovery that you were expecting. Chances are you’ll have your suspicions reaffirmed by your dentist during your follow-up appointment. A failed dental bone graft is sometimes a “watch and wait” type of situation when other times it’s a downward spiral that needs to be tended to quickly.
Sometimes you may not know you have a failed dental bone graft because the gums have healed over it. Your dentist can take a dental X-ray to see if the bone graft material has integrated or not. Integration is where the graft attaches to the adjacent bone and fuses permanently in place. If it hasn’t or it resorbed (dissolved), then you will know that you’ve experienced dental bone graft failure. Signs may just not be visible until your dentist sees the X-ray.
8 Signs Your Bone Graft Failed
Here are the most common things to be on the lookout for:
1. Pain
Some discomfort is normal for 3-4 days after your bone graft surgery. Anything more than that is probably a sign that something is wrong. Soreness is usually normal, but throbbing pain or pain that radiates into other parts of your mouth or throat is not.
2. Tooth Sensitivity
If your graft was placed adjacent to a tooth root (maybe you have periodontal disease and your dentist is trying to save it, or you’re about to get a dental implant in that space) your tooth may be what feels uncomfortable. Especially if there is some type of infection. This type of tooth sensitivity may feel more like an ache or soreness.
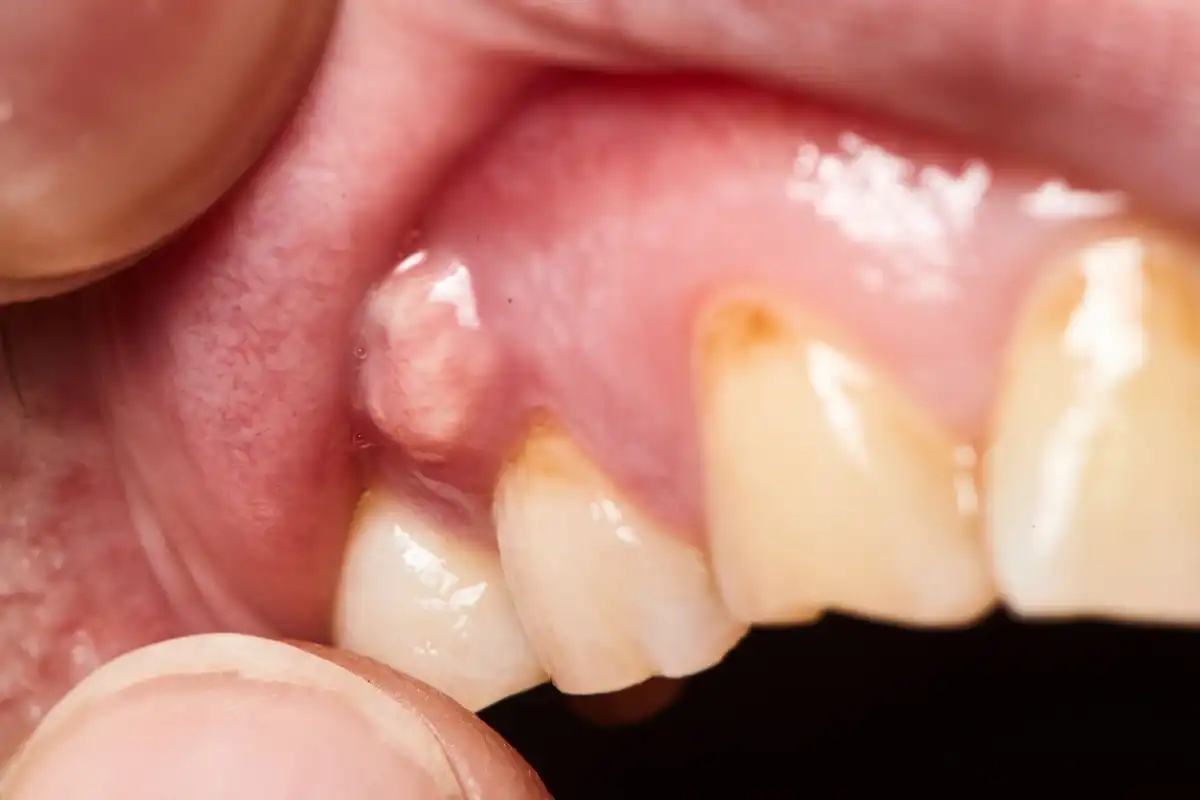
3. Swelling
Gum inflammation is one of the most common symptoms of a failed bone graft. The tissue at that area may mirror gingivitis or periodontitis symptoms, with red, puffy, or bleeding gums. Some minor inflammation is normal for the first few days. But any swelling that doesn’t improve—especially if you’re taking your medication as directed—may mean an infection.
4. Discharge
If there is inflammation, there may also be pus or some type of drainage. And usually, if there is discharge, there will be some type of a sour or salty taste. The fluid may look clear, or it could have a white, milky-like color to it. In some cases, there may be visible bleeding or a black or red hue to the discharge. Green and yellow drainage may also be present.
5. Gum Recession
Your gum tissues rest directly on top of the bone that’s underneath them. So, if you experience bone loss, the receding gums will also start to shrink back. In the case of a bone graft or ridge augmentation, your gum tissues should feel fuller and higher at those points in your mouth. If you experience the gum shrinking or feeling shorter/thinner than before, the graft underneath it may have failed.
6. Sinus Problems
Have you had constant “allergies” since your bone graft was placed? Do you always have a runny nose or a bit of a sinus headache? Did your physician diagnose you with a sinus infection or sinusitis? It might actually be due to an infection where your nasal sinus lining has ruptured at the point of your bone graft site.
7. Irregularities In Your Routine Dental X-Ray
Maybe you don’t have any physical symptoms whatsoever, but your dentist takes a dental X-ray and things just don’t look right. When you look at the before and after X-ray of your bone graft, the graft may be completely dissolved, partially missing, or the shape of the bone has changed in that part of your jaw.
8. Bone Tissue Falling Out
Any time there is loose bone or tiny bone fragments in your jaw, they can work their way out through your gum tissues. We frequently see this after surgical extractions like wisdom tooth removal. In this case, the actual dental bone graft may have just not stayed put.
Reasons Why It Failed
Even though failed dental bone graft treatments are rare, we can usually tie them back to one of the following reasons:
1. Poor Aftercare
Did you follow the home care instructions that your dental office provided? Don’t try to cut corners! If it says not to smoke, don’t. Avoid crunchy foods? Absolutely. Just because one person may have gotten away with it doesn’t mean you should try. Clean your mouth and take your medication as directed.
2. Clenching
Excess pressure on your gums can displace sutures and maybe even your bone graft. People who tend to clench and grind their teeth often may want to sleep in a soft night guard or mouth splint while their mouth is healing.
3. Infection
The most common reason why dental bone grafts fail is because of infection. When your gums and bone are infected, it places everything around it at risk. It could be an infection from dental plaque or more than likely, a sinus infection because of leakage through your sinus lining.
4. Low Blood Flow
Poor blood circulation can cause any type of surgical site to heal poorly. There’s a possibility that your blood vessels were accidentally injured, making it impossible for your body to get the healing nutrients it needs in that area of your mouth.
5. Poor Dental Hygiene
If you’re someone who doesn’t brush or floss as much as you should, bacterial deposits can infect adjacent teeth or even spread into your bloodstream. Without proper oral hygiene, after your bone graft is placed, you may induce your own oral infection.
6. Trauma
A physical injury to your surgical site is a reasonable cause for a failed bone graft. That’s why your dentist will want you to avoid eating hard foods or even cleaning that space with an electric toothbrush or water flosser. Crunchy foods or food that could burn your mouth (like pizza or hot soup) need to be cut out of your diet for several days.
7. Rejection or Absorption
Sometimes our bodies don’t accept graft materials like bone tissue. If your body begins to reject a graft, it will usually shrink away because it hasn’t integrated with the bone around it. Sometimes complete absorption is seen, where the bone essentially dissolves and goes away by itself.
8. The Technique Your Dentist Uses
Not all dentists are trained the same way as oral surgeons, periodontists, or other dental specialists. Even if your dentist is familiar with bone grafting, they could potentially use a technique that doesn’t work quite as well as what might be offered at a specialty clinic where there is more technological support. That’s not to say general dentists can’t place grafts, because they can, but your complex augmentation procedures are probably always going to be referred to a specialist.
When Should I Feel Bone Graft Rejection Symptoms?
Usually, you’re only going to feel sore after a bone graft for about 3-4 days. If pain lasts much longer than that, there may be a complication. Especially if it is chronic throbbing and you cannot eat or swallow comfortably.
Typically, most failed dental bone graft symptoms will be most noticeable within about a 3-4 month timespan. But that’s not going to be the case for everyone. It’s fairly common for it to be several months, a year, or even years later before any type of bone graft failure is observed. Ultimately you want to make sure you care for the graft site as best as possible. Make sure your mouth is healthy and clean so that the site heals well.
Keeping regular checkups every six months is a good idea to monitor the integration of your bone graft. A small X-ray at periodic intervals will allow you and your dentist to visually inspect the area to make sure everything looks as it ought to.
If for any reason you still feel symptoms of pain or swelling after 3-4 days of the graft being placed, it’s best to see your dentist. Even though it can take a few months for the graft to “take”, you should be in the clear of any discomfort after a week or so at the most.
Bone Graft Surgery Retreatment
Fortunately, it’s possible to re-treat a failed dental bone graft procedure. Since the infection is typically the result of an infection—such as sinusitis—your dentist can go in and provide soft tissue therapy at that location to eliminate the source of the bacterial cross-contamination. For example, if the infected area is because of a recent sinus lift procedure and you developed a sinus infection that’s keeping the graft constantly irritated, your dentist can reoperate at that site and place you on medication to manage and prevent another bone graft failure.
- Normally the retreatment process will involve:
- Numbing the area of your mouth where the graft was placed.
- Making a small incision in your gums to open up the graft site.
- Drainage of any infection in that location.
- Prescribing antibiotics.
If necessary, the area can also be cleaned out and new bone grafting material placed in that area. Your dentist may recommend a different type of grafting material, depending on the circumstances regarding your graft failure or rejection.
Some dentists also use PRF (platelet-rich fibrin) or PRP (platelet-rich plasma) in the area of your graft. Both PRP and PRF are proven to help speed up healing times and improve the success of various oral surgeries. However, not all dentists or specialists offer PRP or PRF, so you’ll want to ask your provider.
Sometimes grafting materials are also held into place in your jaw with physical methods like pins or a type of mesh. Once your dentist is happy with how things look, they will place small sutures in the gums to re-cover that area so that it can heal.
Since retreatment rates for bone grafting are highly successful, you can usually expect this graft and surgical site to heal within a few months.
Bone Graft Surgery Cost
| Dental Bone Graft Type | Average Cost |
|---|---|
| Simple Graft using Cadaver, Cow, or Synthetic bone | $200 - $1,200 |
| Bone Graft using Paitnet's own bone (two surgical sites) | $2,000 - $3,500 |
Additional Bone Graft Cost
| Additional Procedures | Additional Cost |
|---|---|
| Panoramic or full-mouth X-Rays | $60 - $250 |
| CT scan | $250 - $1,000 |
Fortunately, if you have a failed dental bone graft and your dentist needs to treat it, they may not need to take the bone out or replace it. It could simply be a matter of handling the infection with medication and cleaning out that area. Your dentist may or may not need to charge a fee. However, if they need to perform full re-treatment including placing a new bone graft, they will probably have to file a dental insurance claim to help pay for the medically necessary procedure.
Complications After Dental Bone Graft
With good home care and taking any medications as prescribed, you can reduce your chances of a bone graft complication. For instance, do not eat anything hard, hot, or spicy early on. And do not vigorously rinse out your mouth or clean your surgical site with a water flosser or electric toothbrush. Too much stimulation—even if it’s just from biting pressure—could lead to complications.
Some types of complications originate back to how the graft was placed, or if the sinus lining drops and allows an infection like sinusitis to cause constant irritation to your graft site.
Infections are probably the most common bone graft complication that we see in dentistry (with many of them related to grafts in the top of your mouth, because of their proximity to your nasal sinuses.) If your dentist puts you on an antibiotic, be sure to take it for the full course of the prescription until the final dose is complete.
Bone Graft Alternatives
PRF and PRP are almost identical when it comes to how the treatment is performed. When you arrive for your appointment, someone will draw a vial of blood from your arm, similar to when you have lab work done. Next, the vial is placed in a machine that separates your blood platelets and fibrin. From there, that part of your plasma or fibrin is then injected or physically placed into the surgical site that your dentist or surgeon has opened up near your jaw. The PRP or PRF—which has a jelly-like texture—is set onto the bone and the gums are sutured closed over it.
When To Talk To A Dentist
If you notice anything outside of the normal symptoms of oral surgery, you need to talk to your dentist. Most dental offices will give you written home-care instructions (post-op instructions) to follow, especially since verbal instructions are easy to forget. Follow your prescribed home care routine properly. But if you start to experience symptoms that are getting worse—such as bleeding, a fever, or pain—especially within 3-4 days after your procedure, pay close attention to the next day or two. Are things better? The same? Worse? If they aren’t better especially within 4-5 days, make sure to touch base with your dentist. They may need to see you back before a full week has passed to intercept an infection or complication. Waiting too long might allow the infection to get worse, leading to additional pain and discomfort.
Most dentists or specialists who perform oral surgeries such as bone grafting will give you an after-hours phone number to call if you need assistance. If you get to the point where you can’t go about your normal activities after a few days, try to call the office during business hours. But if it’s over the weekend or the first day or two after your appointment and you’re in pain or have an obvious infection, do not hesitate to reach out. Your dentist wants you to!
Signs of Dental Bone Graft Failure
Failed dental bone graft treatments are rare. They’re usually a straightforward procedure that’s readily accepted by your body. But sometimes infections develop or your sinuses cause problems. Watching for dental bone graft failure signs in the first several days after your procedure is important. However, some symptoms may never become evident until months or even a year later. Be sure to see your dentist regularly for intermittent exams and X-rays to ensure your graft is “taking” properly. If you do need a bone graft retreatment, the success rate is extremely high. Always be sure to follow your home care instructions carefully, as certain lifestyle habits or mistakes could inadvertently lead to a failed bone graft.
Make your inbox smile!
Subscribe