5 Signs Your Tooth Is Dead & What To Do About It

Every tooth has a “pulp” inside of it made up of nerve tissues and blood vessels. Your pulp feeds your tooth and helps keep it alive. But sometimes, tooth nerves can die. Dead or dying tooth symptoms can be hard to spot right away, but they’re typically different than your run-of-the-mill toothache. Understanding what to watch for—and dead tooth treatment options available—can help you reduce your risk of losing your tooth altogether.
5 Signs Of A Dead Tooth
You might be thinking, “Isn’t it going to be obvious if I have a dead tooth?” Not always. Dying or dead tooth symptoms tend to creep up verrrrrrrrry slowly and happen over a course of weeks, months, or even years in some cases! Then again, there are scenarios where a specific traumatic event could cause immediate tooth death and you’ll know right away.
1. Discolored Tooth
One of the most obvious dead tooth symptoms to watch for is the tooth changing color. Compared to the healthy teeth on either side of it, a dead tooth will usually start to turn brown, grey, or even a bluish color. This color-changing process is because of the dying nerve tissues in the middle of the tooth.
It can take years—sometimes even a decade or more—for a dying tooth to start turning colors. It’s not uncommon for someone to have a sports injury, such as a hit to their mouth with a baseball, where their front tooth doesn’t turn colors until several years later. Suddenly the tooth starts to look bluish or grey when its neighbors don’t; this symptom is a classic tell-tale sign of a dying tooth.
2. Tooth Pain
Even though a dying tooth doesn’t necessarily have a great, healthy, functioning nerve inside of it, it’s still possible for the tooth to feel pain at times. A chronic toothache—whether it be a dull soreness or sharp, intense pain—could indicate that you need dead tooth treatment. Sometimes tooth pain particularly flares up whenever hot temperatures are applied to the tooth, like if you drink a cup of coffee or bite down into hot mashed potatoes. Heat sensitivity is never, ever a good thing.
3. Bad Breath
Whenever a tooth starts to die, you have necrotic (dying) tissues in or around it. We frequently see this with severe cases of periodontal disease, where severe halitosis (bad breath) starts to kick in and practically nothing can get ahead of it. The same thing can happen if you need dead tooth treatment.
Necrotic tissues tend to have a foul, rotten taste and smell to them. Because, well, they’re dying or already dead. If the nerve inside your tooth is dead, it’s not unheard of to have a bad smell coming from it.
4. Bad Taste In Your Mouth
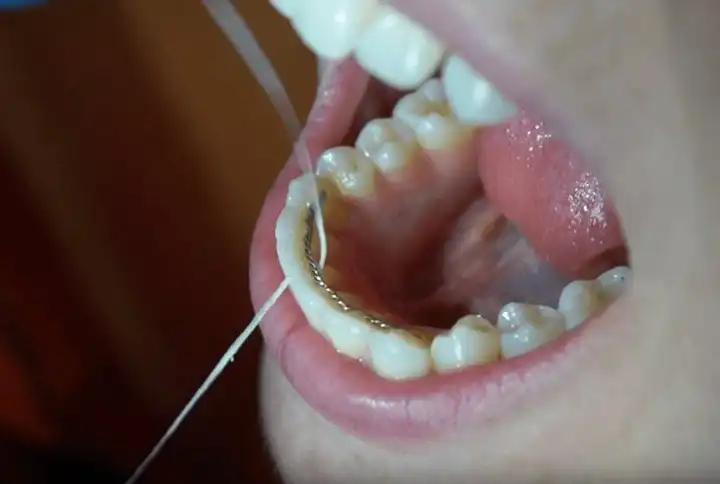
Do you occasionally notice a salty or sour taste in your mouth? Does it seem like the bad taste is coming from one specific area? Maybe you can’t even pinpoint which tooth it’s coming from, but it’s definitely there somewhere and you can tell by running your tongue over it. Chances are, that bad taste is coming from an abscess down inside the gums that you can’t see.
To make sure the bad taste isn’t coming from food or plaque wedged down between your teeth, try running a piece of floss with a small knot it in between the teeth in that area. If you’re not pulling out any food debris, the bad taste is probably from bacteria or a dying tooth.
5. Swelling Around Tooth And Gums
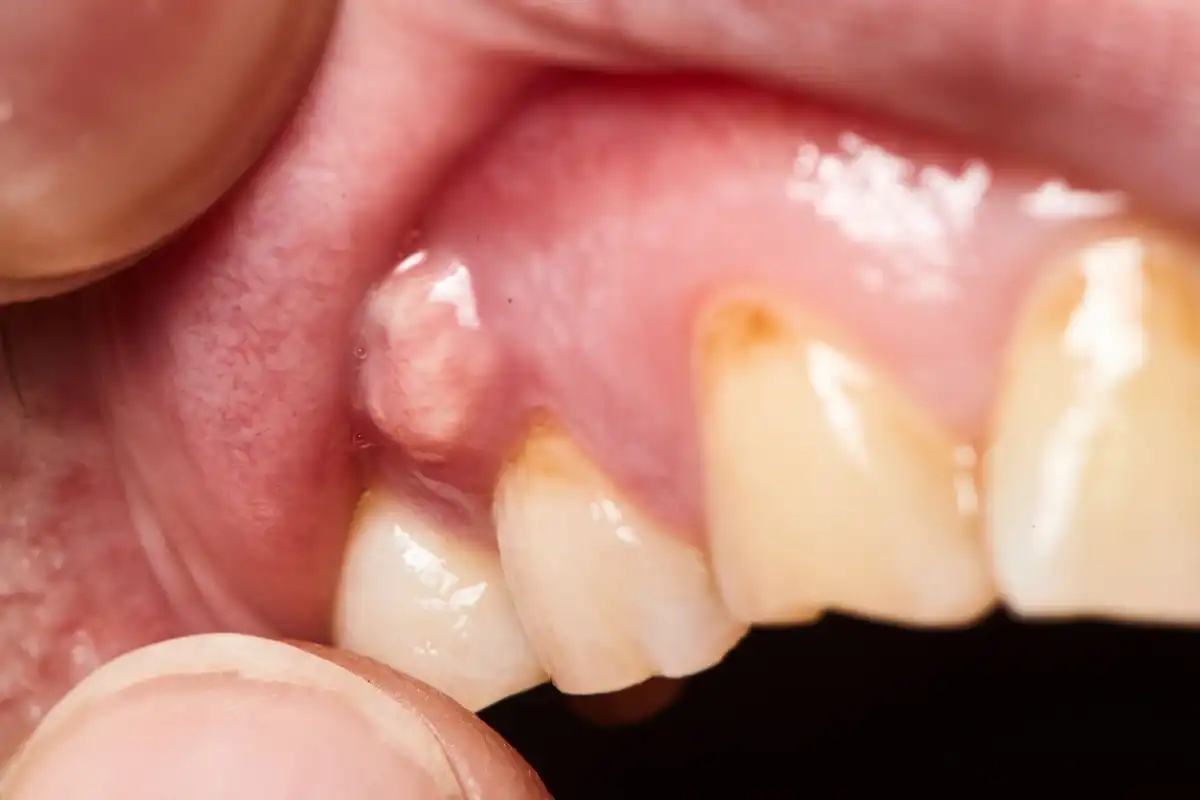
A dead tooth may show signs of abscessing along the gum line just next to the root tip. So, a little further away than the edge of the gums, but somewhere near that specific tooth. A pimple-like “fistula” can develop. This blister-like sore may swell up, drain, go away, and then come back again.
Anytime you see a fistula or mouth swelling around a specific tooth, you need to tend to it quickly. Although it’s rare, abscessed teeth don’t just cause dead tooth symptoms, they can lead to life-threatening infections in your brain. Don’t dismiss it just because the swelling is currently isolated to one tooth.
What Causes A Tooth To Die?
Dying teeth usually result from some issue like untreated dental disease or a traumatic injury. Random, sporadic tooth death isn’t typically something you’re going to see. Chances are, you can put your finger on the cause of your dead tooth and remember the day and time it happened or at least link it back to a specific issue that you already knew about.
Tooth Injury
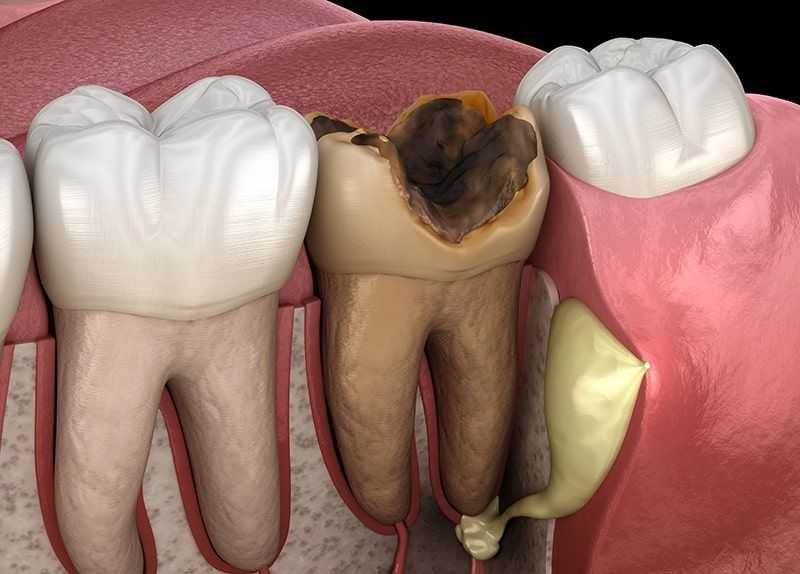
Tooth Decay
Poor dental hygiene can lead to rampant tooth decay and expand into surrounding teeth until the cavities are finally removed by your dentist. Without dental treatment, an untreated cavity can “eat through” your tooth until it finally reaches the nerve inside of it. At that point, the pulp becomes compromised and will start to die. That’s why it’s always best to treat cavities and tooth decay when they’re still small. Over time, these decaying teeth can break down and break off at the gums, only leaving the tooth root intact, exposed nerve and all.
How To Treat A Dead Tooth
You have one of two options for dead tooth treatment: a root canal or removing it altogether. Ideally, the best thing to do is to try to save your natural tooth. Preserving your tooth—as opposed to pulling it—prevents the need for additional treatments related to tooth replacement. It’s typically better and more cost effective to save natural teeth, at least in most situations.
Your dentist will talk to you about what your options are. If the tooth is too damaged, a root canal might not even be an option. But if you’re in severe pain or the infection is getting out of hand, a fast extraction may be your only choice.
Root Canal Treatment
Endodontic therapy (root canal treatment) has a bad reputation. It’s meant for relieving tooth pain and saving teeth, not causing you excruciating pain for days after the procedure. Think of it like getting a filling, except the filling goes down inside of the nerve chamber rather than just a cavity in the top of your tooth. During a root canal the dead nerve remnants is removed, the empty nerve chamber is cleaned out, medication might be placed, and the canal is filled in to prevent any re-infection to the tooth.
A root canal prevents your tooth from breaking down from the inside out. After endodontic treatment, you’ll also need a crown on top of that tooth.
Tooth Extraction
When your tooth is so deteriorated or you’re experiencing over-the-top pain, an emergency dental extraction is typically best for dying teeth. Especially if there’s no way for your dentist to build the tooth back up with a crown. Removing it will prevent the dying tissues from infecting adjacent structures or bacteria from spreading into your face.
Just remember that when you remove a tooth, you also need to replace it. Open spaces in your bite can cause adjacent teeth to start shifting out of alignment. The earlier you replace your tooth the better.
Related: Root Canal vs Extraction: Which is the best option?
How To Prevent A Dead Tooth
1. Wear an athletic mouth guard
If you’re involved in any type of sport that could possibly result in an orofacial injury, make sure you’re wearing a properly fitted mouthguard. Not only will it help against dental trauma, but it can also lower your chances of a concussion.
2. Homecare
Make sure you’re brushing and flossing (or water flossing) each day. Pay close attention to between each tooth and along the edges of the gum tissues, where bacteria tend to be the heaviest. Practice good oral hygiene by brushing twice a day and using fluoride toothpaste.
3. Regular cleanings and checkups
Routine dental appointments allow a dentist or dental hygienist to routinely monitor each tooth and can intercept minor issues like small cavities well before they work their way into the nerve of your tooth.
Talk With Your Dentist About Dead Tooth Concerns
Dying teeth can’t be brought back from the dead. The only thing to do is treat the tooth with a root canal while you still have the tooth or get your dentist to extract it. If you suspect that you’re experiencing dead tooth symptoms, it’s important that you talk to your dentist as quickly as possible. Otherwise, your tooth will eventually reach the point of no return—or you’ll be in pain—where there are no other choices than pulling it.
Dental Insurance can be tricky, ask your dentist about what is covered if you need a root canal or tooth extractions. Dental savings plans are a good way to save if you don't have dental insurance to help pay for dental care.
Dead or Dying Tooth Recap
Dead tooth symptoms frequently include things like discoloration, pain, heat sensitivity, swelling, or a bad taste in your mouth. Dying teeth either need to be treated with a root canal or physically extracted to prevent the spread of infection into your face. If you’re experiencing any symptoms, be sure to talk to your dentist about possible dead tooth treatment.
Make your inbox smile!
Subscribe