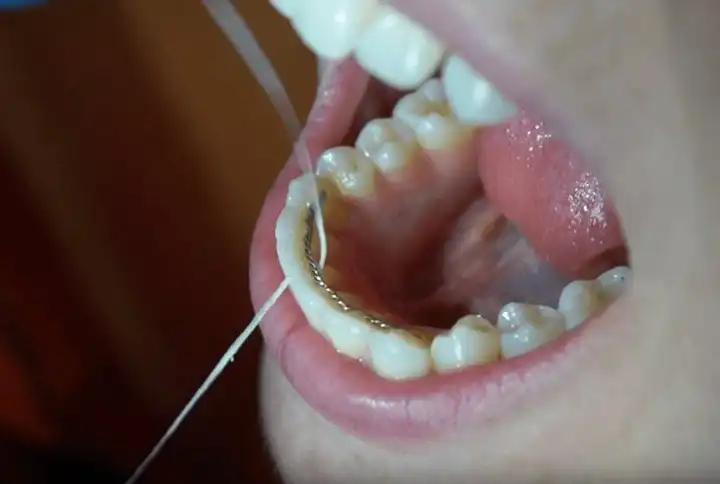
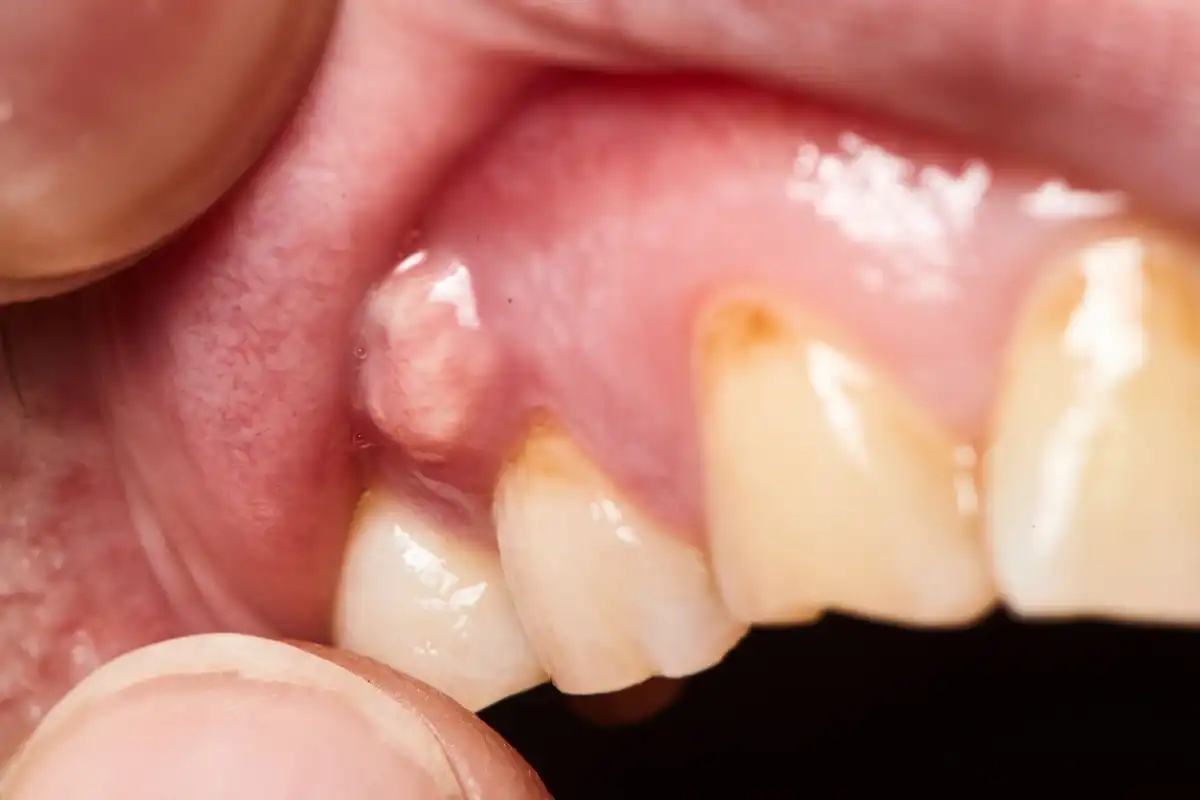
8 Signs of Trench Mouth & How To Get Rid Of It


Trench mouth is a serious oral infection that is known for causing severe pain, inflammation, and ulceration in the gums. It's also called "Vincent's angina" or "acute necrotizing ulcerative gingivitis" (or "ANUG" for short.) The main cause of trench mouth is a bacterial infection, but it can also be triggered by poor oral hygiene, high levels of stress, a history of smoking, and other underlying medical conditions such as HIV or AIDS. Trench mouth can lead to tooth loss if left untreated, so it's important to see a dentist or periodontist as soon as possible if you suspect you have this oral infection.
What Is Trench Mouth? (Acute Necrotizing Ulcerative Gingivitis)
Why is trench mouth called "trench mouth" at all? Because the oral infection was extremely common in soldiers who spent their time in the trenches during World War I.
Trench mouth is like periodontal disease (gum disease) but times 10. Not only do you have swelling, bleeding gums, and bone loss, but you also suffer from ulcerations and things like pus/drainage to deal with. This is not your average gum infection!
How Do You Get Trench Mouth?
Today, some people call periodontal disease "trench mouth," but it's not really the same thing. People with ANUG usually have some sort of underlying health issue on top of their infection, causing it to spiral out of control. Such as:
- Poor diet or malnutrition
- Underlying health conditions such as immune system diseases
- Inadequate or poor dental hygiene
- High levels of psychological stress, as seen in times of war or domestic abuse
8 Signs And Symptoms Of Trench Mouth
You might think that trench mouth looks like your classic case of gum disease. But it's actually much more severe than your typical periodontal infection. And remember, it usually affects young adults who wouldn't otherwise be dealing with periodontitis at their age. They should be in the prime of their life; if they did have poor oral hygiene, the only thing a dental team would expect to see is some really bad gingivitis and tartar buildup. But this is trench mouth we're talking about.
Most people with ANUG will exhibit at least four or more of the following trench mouth symptoms, if not all of them when the infection is severe:
1. Painful, swollen gums
Trench mouth can cause excruciating gum pain. The gum tissues will look bright red and extremely swollen. They may even have a bluish or purple color to them, depending on the severity of the inflammation. Touching them, much less brushing them, causes immediate pain.
Treatment
Even though it hurts to touch your gums, if you have trench mouth, you'll have to touch them to clean them. W arm salt water rinses can ease the pain of inflamed gums. Your dentist or dental hygienist will use local anesthetic to numb the entire area so that they can thoroughly clean each tooth and eliminate the bacterial deposits responsible for the inflamed gums. Since your mouth will be numb during the process, you won’t have to worry about the cleaning being painful.
2. Bleeding gums
The bleeding from trench mouth is typically worse than anything you'll see when it comes to gum infections or gingivitis. Not only will your gums bleed if you brush and floss, but there's also a good chance that you'll have spontaneous bleeding or bleeding when you're biting into or chewing food.
Treatment
To get rid of bleeding gums, your dentist will need to address the source of the bleeding: the bacteria underneath the gum tissues. By cleaning these spaces and putting you on a prescription mouth rinse, along with a good oral hygiene routine, you can typically expect the bleeding to start to improve within a couple of weeks. Daily brushing and flossing are key!
3. Mouth sores
Treatment
For temporary relief, rinse with a warm saltwater mixture throughout the day and take an over-the-counter anti-inflammatory drug such as Motrin. But the only way to permanently treat and get rid of these mouth sores is to see your dentist. Your dental team will likely perform a deep cleaning as well as prescribe antibiotics to reduce the bacterial load in your mouth.
4. Foul breath
Practically nothing causes as bad of breath as gum disease does. Because trench mouth is an aggressive and severe oral infection, your halitosis symptoms are likely to be even worse. In addition to the smell, you might also have bad taste in your mouth because of all of the bacteria, bleeding, and necrotic (dying) tissues deep down around the roots of your teeth.
Treatment
One of the key ways to combat bad breath or ongoing halitosis is by treating the underlying cause. In this case, it's addressing the aggressive gum disease that's infecting the tissues that support the teeth. Your dentist or dental hygienist will need to physically clean around your teeth and under the gum tissues to remove the odor-causing bacteria. Some of the necrotic tissues in these spaces may also be removed during the deep cleaning process. Once the source of the infection is removed, the cycle of necrotic tissue and malodor is stopped or at least improved significantly.
Since the odor originates under your gums, things like breath mints or rinses won't be very helpful. In fact, it could even make your halitosis worse. Especially if your gums or mints contain sugar or the mouth rinse is alcohol based.
5. Difficulty swallowing
Whenever we swallow, we use everything from our tongue to our teeth. Swallowing creates pressure throughout the mouth, which can hurt if your gums have ulcerations across them. On a related note, difficulty swallowing may also be caused by enlarged tonsils and lymph nodes throughout the neck due to the severity of your oral infection. Because you need to be able to eat healthy foods if you have ANUG, problems swallowing can pose an additional layer of concern since most people will shift to a soft, processed diet.
Treatment
Anyone who has trouble swallowing because of an oral infection needs to see their dentist or a dental specialist, such as a periodontist. Difficulty swallowing can be addressed by prescribing medication along with performing a professional cleaning. Additionally, it can be helpful to gargle with warm salt water to help reduce inflammation in the back of the mouth. But things like swollen lymph nodes because of a trench mouth infection typically require antibiotic therapy or similar prescription drugs.
If your throat is so swollen that you're unable to eat, drink, or breathe comfortably, go to the nearest hospital emergency room for immediate attention.
6. Fever
One of the ways our body fights off infection is by raising our internal temperature. People with trench mouth commonly experience at least some type of low-grade fever because of their chronic infection. Because trench mouth is a long and steady infection—rather than something acute with a fast onset—any fevers tend to be low and more prolonged, rather than something that spikes up suddenly. While we don't normally see fevers with traditional periodontal disease, this isn't your average gum infection. The severity of ANUG infections strains your entire body, and your immune system will do whatever it can to protect you.
Treatment
Over-the-counter medications such as ibuprofen or Motrin can help lower your fever as well as help with swelling. But they won't get rid of the bacteria that's causing your fever to flare up in the first place. Make sure you see a dentist or periodontist immediately; they can prescribe stronger medications and plan a debridement or deep cleaning to at least jump-start your body's ability to recover. Simply addressing the symptoms of your fever with drugstore medications will not improve the situation and will only allow it to get worse.
7. Swelling in the face
Aggressive periodontal infections typically cause chronic swelling in the gums immediately around those respective teeth. But with ANUG or trench mouth, the infection can also cause generalized spreading throughout the mouth, face, and neck. You or your medical provider may also note swollen lymph nodes because of the severe level of bacterial infection that's present.
Treatment
Inflammation is NOT cool, especially when it involves your face and/or airway. Your dentist will likely need to prescribe a round of strong antibiotics to start off with, then schedule a cleaning to remove the majority of the bacteria from around your teeth.
If your facial swelling is severe or it's difficult to breathe, head straight to your nearest emergency room. You might need IV antibiotics and steroids to prevent a more serious medical emergency.
8. Fatigue
People with trench mouth typically don't feel well and experience at least some varying degree of fatigue. This is because the body is working hard to fight off the infection, which can take up a lot of energy. Additionally, the pain and discomfort caused by trench mouth can make it difficult for people to eat, sleep, and carry out their daily activities, all of which can contribute to feelings of exhaustion on a day-to-day basis.
Treatment
As your oral infection is treated through deep cleanings and antibiotics, you'll start to notice that you generally feel better as a result. Especially when you're more comfortable eating and sleeping, which will naturally boost your energy levels.
Risk Factors & Complications
Trench mouth is a serious oral infection, and it can have some major, permanent complications if left untreated. Untreated trench mouth can cause tooth loss, weight loss, dehydration and in severe gum infection cases, can cause oral gangrene. Oral bacteria from trench mouth can spread to other parts of the body, similar to traditional periodontal disease.
If you're the victim of abuse, have undergone high levels of psychological or physical trauma, or know that you have an underlying medical condition such as HIV/AIDS or diabetes, these factors can increase your chances of developing trench mouth.
Severe oral infections like these can also make it difficult to eat or speak due to the pain, inflammation, and ulceration in your gums. Not to mention the self-consciousness caused by the odor it puts off.
It's important to see a dentist or periodontist as soon as possible if you suspect you have trench mouth, as early treatment can help prevent these complications and help you to recover more quickly.
How To Treat Trench Mouth
Your dentist will probably recommend a periodontal treatment plan that also includes antibiotics due to the severity of the bacterial infection. Most people with gum disease do not need antibiotic treatment, but trench mouth is different.
More than likely, your trench mouth treatment will begin with an antibiotic regimen before your upcoming dental treatment, which typically includes a series of deep cleanings (scaling and root planing.) After your deep cleaning, your dentist may also prescribe a heavy-duty mouthwash such as chlorhexidine or locally placed antibiotic capsules under specific areas of gum tissue. If tissue detachment is severe, some teeth may need to be extracted.
Does Trench Mouth Go Away?
How To Prevent Trench Mouth
Trench mouth is an aggressive periodontal infection that can be prevented by maintaining good oral hygiene practices, a balanced healthy diet, and hopefully a low-stress lifestyle.
- Here are a few ways you can help prevent trench mouth from happening:
- Proper oral hygiene, brush and floss your teeth regularly to remove plaque and bacteria from your mouth.
- Use an antiseptic mouthwash after brushing and flossing.
- Schedule regular dental check-ups and dental cleanings to keep your teeth and gums healthy.
- Address risk factors such as smoking, nutritional deficiencies, or medical conditions like HIV/AIDS with the help of your medical provider.
- Manage stress levels (when possible, that is!)
Remember that in dentistry, prevention is always better than a cure, so don't hesitate to visit your dentist if you have any concerns about your oral health.
Talk With Your Dentist
Trench mouth or acute necrotizing ulcerative gingivitis (ANUG) is a severe, rare oral infection that affects young adults undergoing serious levels of stress. In many scenarios, these individuals haven't had access to dental care for some reason or another. Fortunately, it's not too late. If you have ulcerative gums and symptoms of an advanced gum infection—along with fever, fatigue, or facial swelling—you need to seek dental care immediately. Consider going straight to a periodontist (gum specialist) or call a trusted family dentist in your area.
Make your inbox smile!
Subscribe